## Clinical Diagnosis: G6PD Deficiency with Acute Hemolytic Crisis ### Key Clinical Features **Key Point:** The combination of acute hemolysis triggered by a known oxidative drug (TMP-SMX), bite cells on blood smear, negative DAT, and African descent ethnicity is diagnostic of G6PD deficiency. ### Diagnostic Reasoning 1. **Oxidative drug trigger** — Trimethoprim-sulfamethoxazole is a classic oxidative stressor that precipitates hemolysis in G6PD-deficient patients 2. **Bite cells on blood smear** — pathognomonic for G6PD deficiency; represent RBCs with Heinz bodies removed by splenic macrophages, leaving a "bite" appearance 3. **Negative DAT** — excludes immune-mediated hemolysis (AIHA) 4. **African descent** — G6PD deficiency is most common in African, Mediterranean, and Asian populations; ~10% of African American males are affected 5. **Acute presentation** — G6PD hemolysis is episodic and triggered by oxidative stress, not chronic 6. **Normal hemoglobin electrophoresis** — excludes hemoglobinopathies (sickle cell, thalassemia) ### Laboratory Pattern in G6PD Deficiency | Parameter | Finding | Interpretation | |-----------|---------|----------------| | Hemoglobin | 6.8 g/dL | Severe anemia from acute hemolysis | | Reticulocyte count | 12% | Markedly elevated, bone marrow response | | Indirect bilirubin | 5.1 mg/dL | Elevated from RBC breakdown | | LDH | 950 U/L | Very high, from intravascular hemolysis | | Haptoglobin | <5 mg/dL | Depleted, consumed by free Hb | | DAT | Negative | **Excludes immune-mediated hemolysis** | | Blood smear | Bite cells + Heinz bodies | **Pathognomonic for G6PD** | | Hemoglobin electrophoresis | Normal | **Excludes hemoglobinopathies** | ### Pathophysiology of G6PD Deficiency **High-Yield:** Glucose-6-phosphate dehydrogenase is the first enzyme in the pentose phosphate pathway, essential for generating NADPH. NADPH maintains reduced glutathione (GSH), which protects RBCs from oxidative damage. G6PD deficiency → ↓NADPH → ↓GSH → oxidative stress → RBC membrane damage → hemolysis. ### Heinz Bodies and Bite Cells **Mnemonic: HEINZ = Hemoglobin Enzyme Inactivation and Neoantigen Zeneration** - **Heinz bodies** — precipitated, denatured hemoglobin visible with supravital stains (brilliant cresyl blue, new methylene blue) - **Bite cells** — RBCs with Heinz bodies partially removed by splenic macrophages, leaving a characteristic "bite" or indentation - These findings are **diagnostic** for G6PD deficiency ### Common Oxidative Triggers | Category | Examples | |----------|----------| | **Drugs** | Sulfonamides (TMP-SMX), aspirin, antimalarials (primaquine), nitrofurantoin, dapsone, sulfonylureas | | **Infections** | Bacterial (UTI, pneumonia), viral (hepatitis A, EBV) | | **Foods** | Fava beans (hence "favism") | | **Other** | Acidosis, hypoxia, strenuous exercise | ### Why Negative DAT Rules Out AIHA Autoimmune hemolytic anemia (AIHA) presents with positive DAT because IgG or complement is bound to RBC surface. This patient's negative DAT excludes AIHA, even though he has spherocytes (which can occur in both conditions). ### Diagnosis Confirmation **Clinical Pearl:** Definitive diagnosis of G6PD deficiency requires **G6PD enzyme assay** (quantitative or qualitative). However, during acute hemolytic crisis, reticulocytosis may falsely elevate enzyme levels (young RBCs have higher G6PD activity), so testing should be deferred 2–3 weeks after recovery. ### Management 1. **Acute crisis** — supportive care, transfusion if Hb <5 g/dL, IV fluids, monitor for acute kidney injury 2. **Discontinue oxidative drugs** — remove TMP-SMX and any other offending agent 3. **Avoid future triggers** — patient education on drugs, foods, and infections to avoid 4. **Folic acid supplementation** — for chronic hemolysis (if present) 5. **No splenectomy** — unlike hereditary spherocytosis, splenectomy does not help in G6PD **Warning:** Do not confuse G6PD deficiency with hereditary spherocytosis. Both can present with hemolysis and spherocytes, but HS has positive osmotic fragility, HS is chronic/recurrent without clear triggers, and HS responds to splenectomy. G6PD is acute/episodic, triggered by oxidative stress, and shows bite cells (HS does not). [cite:Robbins 10e Ch 12] 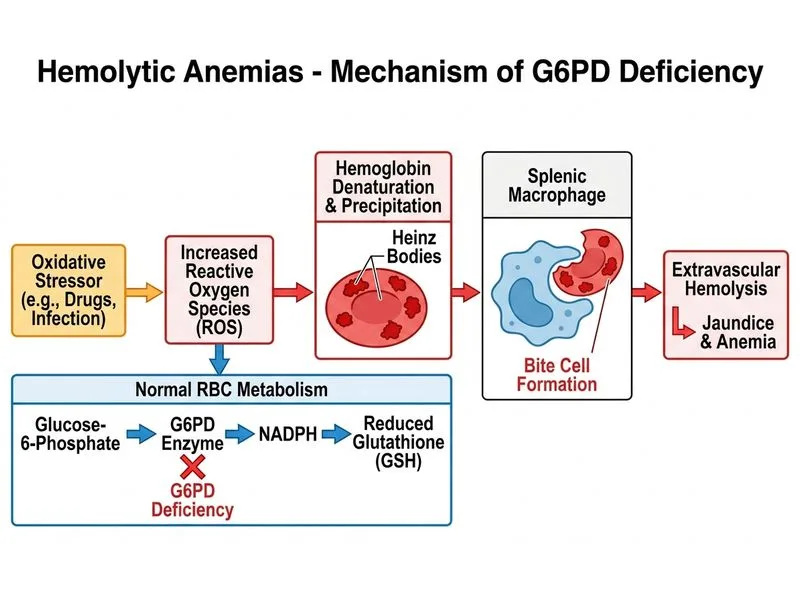
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.