## Clinical Diagnosis This patient has **autoimmune hemolytic anemia (AIHA)** with warm-antibody type, evidenced by: - Positive DAT (Coombs test) — pathognomonic for immune-mediated hemolysis - Spherocytes on smear (antibody-coated RBCs lose membrane) - Elevated indirect bilirubin and reticulocytosis - Low haptoglobin (consumed by free hemoglobin) - Splenomegaly (site of antibody-mediated RBC destruction) **Key Point:** DAT positivity is the diagnostic hallmark of AIHA and distinguishes it from hereditary spherocytosis (which has negative DAT). ## Management Algorithm ```mermaid flowchart TD A[AIHA Confirmed: Positive DAT]:::outcome --> B{Hemoglobin Level?}:::decision B -->|Hb < 7 g/dL or symptomatic| C[Transfuse PRBCs + Start Corticosteroids]:::action B -->|Hb 7-10 g/dL| D[Corticosteroids ± Transfusion PRN]:::action C --> E[Prednisolone 1 mg/kg/day]:::action D --> E E --> F[Response Assessment at 1-2 weeks]:::decision F -->|Responds| G[Taper steroids over 2-3 months]:::action F -->|No response| H[Add Azathioprine or Rituximab]:::action H --> I[Consider Splenectomy if refractory]:::action ``` ## Why This Option Is Correct **High-Yield:** In acute AIHA with Hb 7.2 g/dL (symptomatic anemia) and positive DAT: 1. **Immediate transfusion** is needed to prevent end-organ hypoxia (risk of stroke, MI, acute kidney injury) 2. **Concurrent corticosteroid initiation** (prednisolone 1 mg/kg/day) suppresses antibody production and reduces hemolysis 3. This dual approach addresses both immediate oxygen delivery and underlying immune pathology **Clinical Pearl:** Transfusion in AIHA carries risk of transfused RBCs being hemolyzed, but the benefit of correcting severe anemia outweighs this risk. Use least incompatible blood if possible. **Warning:** Do NOT delay transfusion waiting for splenectomy or additional testing — the patient is symptomatic with Hb <8 g/dL. ## Timeline of AIHA Management | Phase | Intervention | Timing | |-------|--------------|--------| | **Acute (Days 1–3)** | Transfusion + Corticosteroids | Immediate | | **Early (Weeks 1–2)** | Assess response; continue steroids | Ongoing | | **Maintenance (Weeks 2–12)** | Taper prednisolone if responding | Gradual | | **Refractory (>2 weeks)** | Add azathioprine, rituximab, or splenectomy | If needed | **Mnemonic: AIHA Management = TCS (Transfuse, Corticosteroids, Splenectomy if refractory)** ## Why Splenectomy Is NOT First-Line Here Splenectomy is reserved for: - Corticosteroid-dependent or refractory cases (after 2–4 weeks of steroid trial) - Patients requiring unacceptable steroid doses to maintain remission - NOT as immediate therapy in acute presentation Urgent splenectomy in option 1 is premature and inappropriate. 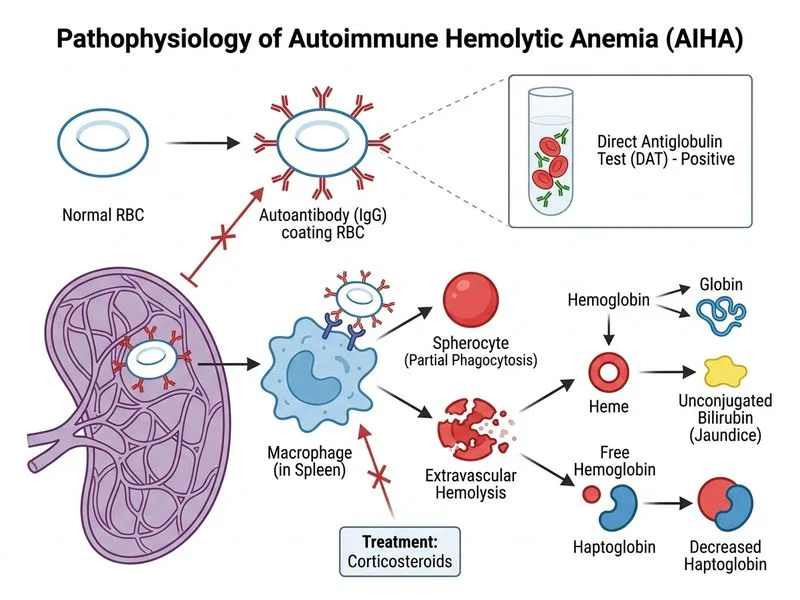
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.