## Pathophysiology of Hypertensive Intracerebral Hemorrhage (ICH) This patient has classic hypertensive ICH in the basal ganglia (putamen/globus pallidus region), which accounts for 35–50% of hypertensive ICH cases. Understanding the **primary** mechanism of neurological deficit is essential for NEET PG/INI-CET. ### Key Point: Primary Mechanism of Neurological Deficit in ICH **High-Yield:** The **primary and immediate mechanism** of neurological deficit in intracerebral hemorrhage is **direct tissue destruction and neuronal loss from the hematoma itself.** The expanding hematoma physically disrupts neural pathways, white matter tracts, and gray matter nuclei at the site of bleeding. In this patient: 1. **Left basal ganglia hematoma (3.5 cm)** — directly destroys the putamen and surrounding structures, interrupting the corticospinal tract (causing right hemiparesis) and cortical-subcortical language circuits (causing expressive aphasia) 2. **Hyperdense lesion on NCCT** — represents acute blood, confirming active hemorrhage with direct parenchymal destruction 3. **Acute onset** — the immediate neurological deficits at presentation are caused by the hematoma itself, not by edema (which takes hours to develop) ### Timeline of Injury Mechanisms | Phase | Timeframe | Dominant Mechanism | |---|---|---| | **Acute** | 0–6 hours | **Direct tissue destruction** (primary) | | **Subacute** | 6–72 hours | Vasogenic edema, hematoma expansion | | **Chronic** | >72 hours | Gliosis, hemosiderin deposition | ### Why Vasogenic Edema (Option B) Is NOT the Primary Mechanism While vasogenic edema and mass effect are important **secondary** contributors to neurological deterioration (peaking at 24–48 hours), they are **not the primary mechanism** of the initial deficit. The patient's acute-onset right hemiparesis and aphasia are directly caused by the hematoma destroying basal ganglia and adjacent internal capsule fibers — this occurs at the moment of hemorrhage, before significant edema develops. The surrounding hypodensity (edema) and 4 mm midline shift represent **secondary injury** that may worsen the deficit over time, but the **primary** neurological deficit is attributable to direct parenchymal destruction. ### Why Other Options Are Incorrect - **Option A (Thromboembolism):** ICH does not cause arterial occlusion; this mechanism applies to ischemic stroke - **Option C (Seizure-induced dysfunction):** No seizure activity is described; Todd's paralysis is a diagnosis of exclusion - **Option B (Vasogenic edema/ICP):** A secondary mechanism that evolves over hours to days, not the primary cause of acute deficits at presentation ### Clinical Pearl **Per Harrison's Principles (21e, Ch. 296):** In ICH, the hematoma causes immediate neurological deficits through direct mechanical disruption of neural tissue. Secondary injury from edema, inflammation, and mass effect compounds the deficit in subsequent hours to days. The distinction between primary (direct destruction) and secondary (edema/ICP) mechanisms is critical for understanding the temporal evolution of ICH. [cite: Harrison 21e Ch 296; Robbins 10e Ch 28; Adams & Victor's Principles of Neurology] 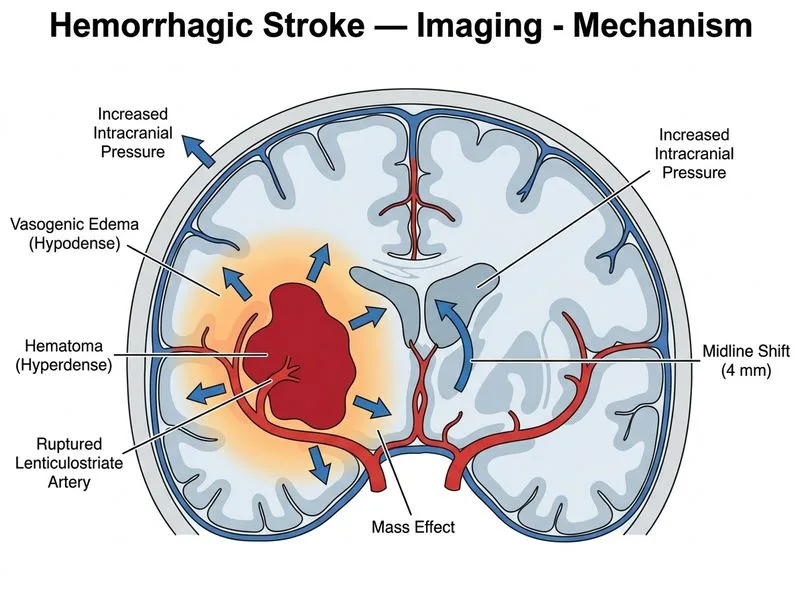
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.