## Imaging Strategy in Hypertensive Intracerebral Hemorrhage ### Clinical Context: Hypertensive ICH vs. Secondary Hemorrhage **Key Point:** While the clinical presentation and location (basal ganglia) are classic for hypertensive ICH, imaging must exclude secondary causes — particularly vascular malformations (AVM), aneurysms, and tumor — before attributing hemorrhage to hypertension alone. ### Why CTA Is Essential Here | Investigation | Indication | Sensitivity | Timing | |---|---|---|---| | **Non-contrast CT** | Detect acute blood, mass effect | 100% for acute bleed | Immediate | | **CT Angiography** | Exclude aneurysm, AVM, tumor blush | 95–98% for aneurysm; 90% for AVM | After diagnosis confirmed | | **CT Perfusion** | Assess ischemic penumbra | Useful in ischemic stroke | Not standard in ICH | | **MRI (gradient echo)** | Detect chronic microhemorrhages (CAA) | Excellent for microhemorrhages | Days later, not acute | | **Repeat CT at 24 hrs** | Monitor hematoma expansion | Prognostic but not diagnostic | Not first-line | **High-Yield:** Current guidelines (AHA/ASA 2015, updated 2019) recommend CTA or conventional angiography in all patients with ICH to exclude secondary causes, especially: - Younger patients (< 45 years) - Lobar hemorrhage (cortical location) - Absence of hypertension or coagulopathy - Atypical imaging features This 72-year-old has hypertension, but the 4 cm basal ganglia hematoma with intraventricular extension and significant mass effect warrants exclusion of underlying vascular lesions before committing to medical management alone. ### Hypertensive ICH: Typical Features **Mnemonic:** **CHAMPS** — **C**audate/basal ganglia, **H**ypertension history, **A**cute onset, **M**ass effect common, **P**utamen/globus pallidus, **S**mall vessel disease (lipohyalinosis). Common locations: 1. Basal ganglia (putamen/globus pallidus) — 50% 2. Thalamus — 20% 3. Pons — 15% 4. Cerebellum — 10% 5. Lobar (cortical) — rare in pure hypertensive ICH **Clinical Pearl:** Lobar hemorrhage in an elderly patient should raise suspicion for cerebral amyloid angiopathy (CAA), which may show multiple microhemorrhages on gradient echo MRI and carries risk of recurrent lobar bleeds. ### Why Each Alternative Is Suboptimal **CT Perfusion** is used in acute ischemic stroke to identify salvageable tissue; it is not standard in ICH management and does not address the need to exclude secondary causes. **Repeat CT at 24 hours** is useful for prognostication (hematoma expansion predicts poor outcome) but does not identify the underlying etiology and delays diagnosis of a potentially treatable lesion. **MRI with gradient echo** is excellent for detecting chronic microhemorrhages (suggesting CAA) but is not the first-line acute imaging study and does not exclude acute vascular lesions as effectively as CTA. ### Management Implications If CTA shows no aneurysm or AVM, management proceeds with: - Blood pressure control (target SBP < 140 mmHg) - Reversal of anticoagulation if applicable - Consideration of surgical evacuation if hematoma is > 3 cm, in accessible location, and patient is surgical candidate - ICU monitoring for hematoma expansion and complications 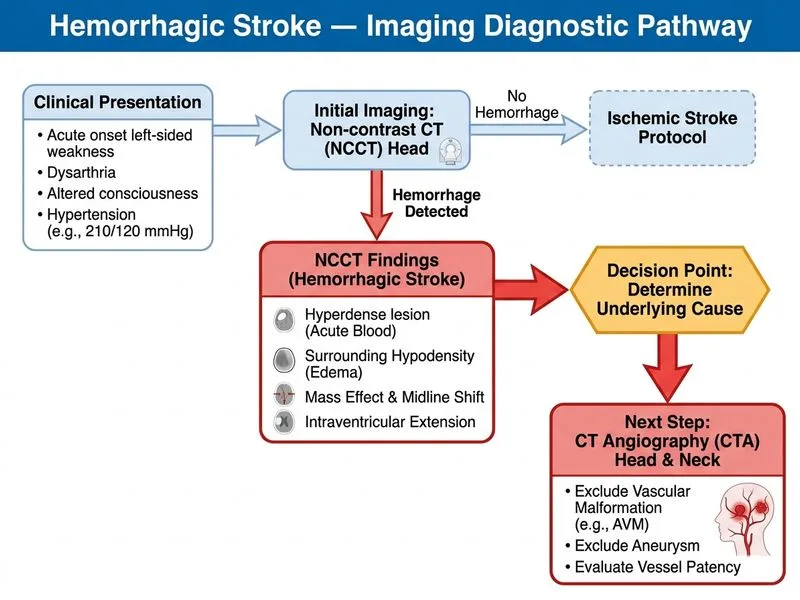
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.