## Clinical Context This patient presents with acute hypertensive intracerebral hemorrhage (ICH) in the basal ganglia — a typical location for hypertensive bleeding. The initial non-contrast CT confirms acute blood (hyperdense) with surrounding edema (hypodensity) and mass effect (midline shift). ## Why CTA is the Next Step **High-Yield:** In acute ICH, CTA of the head and neck is the standard next imaging after non-contrast CT to identify secondary causes and guide prognosis. **Key Point:** CTA serves two critical functions: 1. **Detect underlying vascular lesions** — aneurysm, arteriovenous malformation (AVM), or arteriovenous fistula that may have caused the hemorrhage 2. **Identify "spot sign"** — contrast extravasation into the hematoma indicating active bleeding, which predicts hematoma expansion and poor outcome; presence of spot sign may influence decision for hemostatic therapy or reversal of anticoagulation ## Imaging Characteristics of Hypertensive ICH | Feature | Hypertensive ICH | | --- | --- | | **Location** | Basal ganglia (50%), thalamus (15%), pons (10%), cerebellum (10%), lobar (15%) | | **CT appearance** | Hyperdense (acute), surrounded by hypodensity (vasogenic edema) | | **CTA findings** | Spot sign present in 35% (indicates active bleeding) | | **Underlying lesion** | Lipohyalinosis of penetrating arteries; no aneurysm or AVM | ## Why Other Options Are Incorrect **MRI with GRE/SWI:** While excellent for detecting microhemorrhages and chronic blood products, MRI is not the immediate next step in acute ICH. It is slower, less available in emergency settings, and does not provide information about active bleeding (spot sign) or underlying vascular lesions as effectively as CTA. **Repeat non-contrast CT at 24 hours:** Serial CT is used to monitor hematoma expansion (which occurs in ~30% of patients within 24 hours), but it does NOT identify the cause of hemorrhage or active bleeding. CTA should be done first to guide acute management. **Transcranial Doppler ultrasound:** While useful for detecting vasospasm in subarachnoid hemorrhage, it has no role in the acute assessment of ICH and does not identify underlying vascular lesions. ## Clinical Pearl **Spot sign on CTA** is an independent predictor of poor outcome and hematoma expansion. Its presence may prompt consideration of hemostatic agents (e.g., tranexamic acid, fresh frozen plasma, prothrombin complex concentrate) or reversal of anticoagulation if the patient is anticoagulated. 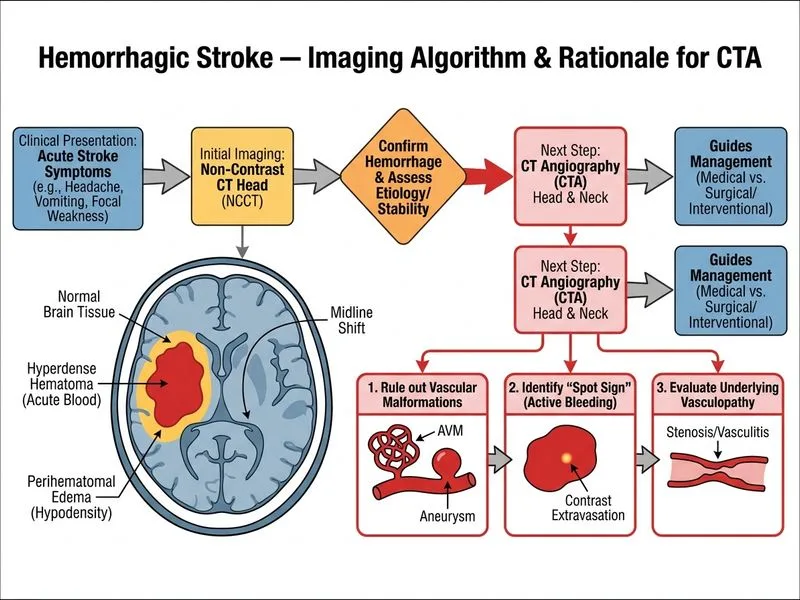
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.