## Clinical Presentation Analysis **Key Point:** The classic triad of sudden severe headache, neck stiffness, and photophobia is pathognomonic for subarachnoid hemorrhage (SAH). The patient's hypertensive presentation (180/110 mmHg) is a common secondary effect of acute intracranial hemorrhage. ## Imaging Interpretation **High-Yield:** Hyperdense material in the basal cisterns and sylvian fissures on NCCT is the hallmark of SAH. The bilateral distribution and location in subarachnoid spaces (not parenchymal) rules out epidural hematoma (which appears as lens-shaped, unilateral, and does not cross sutures) and intracerebral hemorrhage (which is intraparenchymal). ## Diagnostic Algorithm ```mermaid flowchart TD A["Sudden severe headache + neck stiffness + photophobia"]:::outcome --> B["NCCT Head"]:::action B --> C{"Hyperdense in basal cisterns/sylvian fissures?"}:::decision C -->|Yes| D["Subarachnoid Hemorrhage"]:::outcome D --> E["CTA Head & Neck"]:::action E --> F{"Aneurysm identified?"}:::decision F -->|Yes| G["Endovascular coiling or surgical clip"]:::action F -->|No| H["Repeat CTA or DSA"]:::action C -->|No| I["Consider alternative diagnosis"]:::outcome ``` ## Next Imaging Step: CT Angiography **Clinical Pearl:** CTA (CT angiography) of the head and neck is the gold standard first-line vascular imaging after NCCT confirms SAH. It has >95% sensitivity for aneurysms ≥3 mm and is non-invasive, rapid, and widely available. It evaluates: - Circle of Willis and major intracranial vessels - Vertebral and carotid arteries (neck vessels) - Aneurysm location, size, and morphology - Vasospasm (if performed in delayed phase) **High-Yield:** If CTA is negative but clinical suspicion remains high (e.g., thunderclap headache, xanthochromia on LP), digital subtraction angiography (DSA) is the next step — it is more sensitive for small aneurysms and AVM but is invasive and reserved for therapeutic intervention or when CTA is inconclusive. ## Why NCCT Alone Is Insufficient NCCT identifies the hemorrhage but does NOT identify the source. In ~85% of non-traumatic SAH, the cause is a ruptured cerebral aneurysm; in ~10%, it is an arteriovenous malformation; in ~5%, the source is cryptogenic. Vascular imaging is mandatory for treatment planning. [cite:Harrison 21e Ch 297] 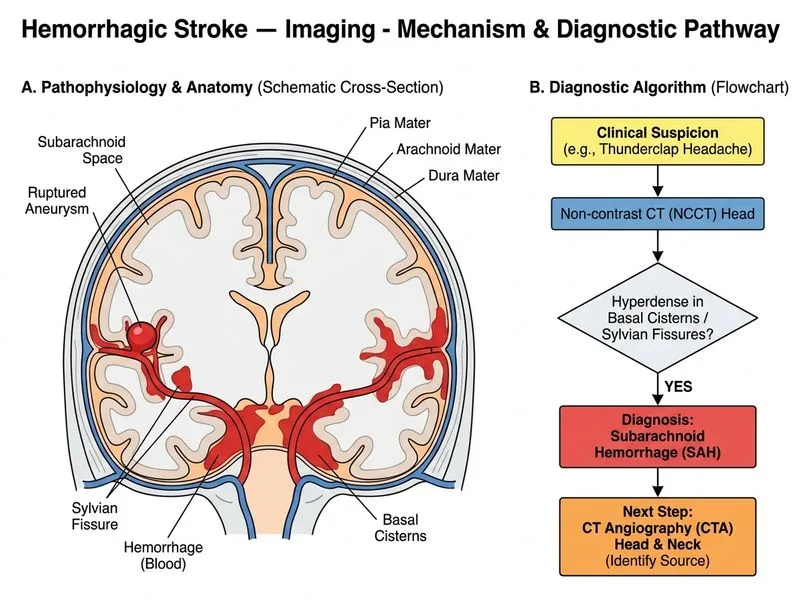
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.