## Imaging Hemorrhagic Transformation in Acute Ischemic Stroke ### Clinical Scenario Analysis This patient has acute ischemic stroke with subsequent hemorrhagic transformation (HT), a serious complication occurring in 10–40% of ischemic stroke cases. The clinical deterioration and imaging findings suggest both hemorrhage and possible thrombus extension, requiring comprehensive vascular and parenchymal assessment. ### Why MRI with SWI and MRA is Correct **Key Point:** MRI with susceptibility-weighted imaging (SWI) and MR angiography (MRA) is superior for characterizing hemorrhagic transformation and assessing vascular patency: - **SWI sequences** are exquisitely sensitive for blood products (hemosiderin, deoxyhemoglobin) and can differentiate hemorrhagic infarction from parenchymal hematoma - **MRA** provides high-resolution visualization of intracranial and extracranial vessels without contrast, detecting thrombus, dissection, or recanalization - **DWI/ADC** (already performed) confirm acute ischemia; repeat MRI adds vascular detail **High-Yield:** SWI is more sensitive than CT for detecting microhemorrhages and blood product evolution, and MRA avoids iodinated contrast (important in renal impairment or contrast allergy). ### Comparison of Imaging Modalities for Hemorrhagic Transformation | Modality | Hemorrhage Detection | Vascular Assessment | Contrast Required | Sensitivity for Microhemorrhage | |---|---|---|---|---| | **NCCT** | Good (acute hyperdensity) | Poor | No | Very low | | **CTP + CTA** | Moderate | Excellent (CTA) | Yes (iodinated) | Low | | **MRI + SWI + MRA** | Excellent (all phases) | Excellent (MRA) | No (MRA non-contrast) | **Highest** | | **Transcranial Doppler** | None | Bedside flow assessment only | No | N/A | **Clinical Pearl:** Hemorrhagic transformation is classified as: 1. **HI-1 / HI-2** (hemorrhagic infarction): small petechial hemorrhages within infarct 2. **PH-1 / PH-2** (parenchymal hematoma): >30% of infarct volume with mass effect SWI is the gold standard for detecting and grading these subtypes. ### Why MRI with SWI + MRA Surpasses Alternatives **Advantages over NCCT:** - NCCT is insensitive to microhemorrhages and cannot assess vessel patency - SWI detects blood products at all stages (acute, subacute, chronic) **Advantages over CTP + CTA:** - CTA is excellent for large vessel occlusion but requires iodinated contrast - CTP assesses perfusion but is less sensitive for hemorrhage characterization than SWI - MRA provides equivalent vascular detail without contrast **Advantages over Transcranial Doppler:** - TCD is bedside but cannot diagnose hemorrhage or visualize parenchyma - Operator-dependent; poor acoustic windows in elderly patients ### Diagnostic Pathway ```mermaid flowchart TD A["Acute ischemic stroke on MRI DWI"]:::outcome --> B["Thrombolysis/thrombectomy?"]:::decision B -->|"Yes"| C["CTA for LVO assessment"]:::action B -->|"No"| D["Monitor clinically"]:::action D --> E{"Clinical deterioration?"}:::decision E -->|"Yes"| F["Repeat imaging for HT"]:::action F --> G{"Characterize HT + assess vessels?"}:::decision G -->|"MRI SWI + MRA preferred"| H["Detect microhemorrhage, grade HT, assess recanalization"]:::action G -->|"NCCT only"| I["Limited hemorrhage detail, no vascular info"]:::outcome H --> J{"Thrombus extension or new occlusion?"}:::decision J -->|"Yes"| K["Neurology/Neurosurgery consult"]:::action ``` **Warning:** Do not rely on NCCT alone for hemorrhagic transformation assessment in the subacute phase; microhemorrhages and small petechial bleeds may be missed, leading to underestimation of HT severity. [cite:Harrison 21e Ch 296; Robbins 10e Ch 28] 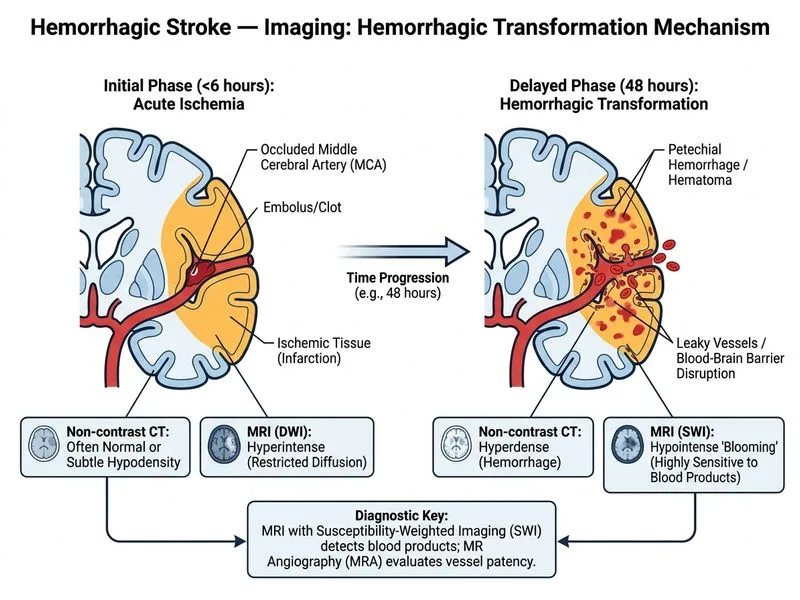
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.