## Clinical Context The patient presents with classic subarachnoid hemorrhage (SAH) symptoms and non-contrast CT confirms blood in the subarachnoid space. The next critical step is to identify the source of bleeding, which is most commonly a ruptured intracranial aneurysm. ## Why CTA is the Best Next Step **Key Point:** CT angiography (CTA) is the current gold-standard first-line imaging modality for detecting aneurysms in acute SAH. It has high sensitivity (95–98%) and specificity (>99%) for aneurysms ≥3 mm and can be performed rapidly in the emergency setting without the need for invasive catheterization. **High-Yield:** CTA provides: - Fast, non-invasive aneurysm detection - 3D reconstructions for surgical/endovascular planning - Assessment of vasospasm risk and collateral circulation - Identification of other sources (AVM, dissection, mycotic aneurysm) ## Timing and Protocol **Clinical Pearl:** CTA should be performed immediately after confirming SAH on non-contrast CT. If CTA is negative but clinical suspicion remains high (e.g., thunderclap headache with negative initial CT), repeat CT in 6 hours or proceed to DSA. ## Role of DSA Digital subtraction angiography is now reserved for: - Therapeutic intervention (coil embolization, flow diversion) - Cases where CTA is inconclusive or contraindicated - NOT as a first-line diagnostic tool in acute SAH [cite:Harrison 21e Ch 445] 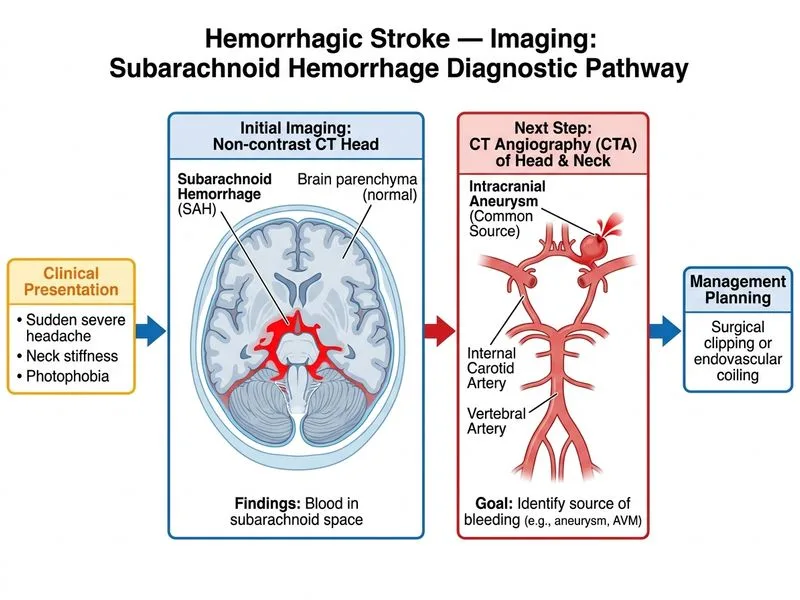
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.