## Clinical Context: Hypertensive Intracerebral Hemorrhage (ICH) **Key Point:** In acute hypertensive ICH, **hematoma expansion** is a critical prognostic factor and occurs in 30–50% of patients within the first 24 hours. Serial imaging is the standard of care to detect expansion and guide intervention decisions. ### Why Repeat CT at 24 Hours? **High-Yield:** Early hematoma expansion (within first few hours) is associated with: - Worse clinical outcomes - Higher mortality and morbidity - Greater disability at discharge - Indication for aggressive blood pressure control and possible surgical evacuation ### Imaging Timeline in ICH | Time Point | CT Appearance | Clinical Significance | |------------|---------------|----------------------| | **Hyperacute (0–6 hrs)** | Hyperdense, well-demarcated | Acute blood; risk of expansion | | **Acute (6–24 hrs)** | Hyperdense with edema | Peak expansion risk; repeat imaging recommended | | **Subacute (1–3 weeks)** | Isodense rim, hypodense center | Edema peaks; mass effect may worsen | | **Chronic (>3 weeks)** | Hypodense; hemosiderin rim on MRI | Resorption phase | **Clinical Pearl:** The **ICH Score** (based on hematoma volume, intraventricular hemorrhage, infratentorial location, and Glasgow Coma Scale) predicts 30-day mortality. Serial CT helps refine this score and detect complications (expansion, hydrocephalus, herniation). ### Management Algorithm for Hypertensive ICH ```mermaid flowchart TD A[Acute ICH on CT]:::outcome --> B{Hematoma volume?}:::decision B -->|< 30 mL| C[Medical management + BP control]:::action B -->|30-60 mL| D[Assess expansion risk]:::decision B -->|> 60 mL| E[Consider surgical evacuation]:::action D -->|Repeat CT at 24 hrs|F{Expansion?}:::decision F -->|Yes + deterioration| E F -->|No + stable| C E --> G[Neurosurgical consultation]:::action C --> H[ICU monitoring, antihypertensive therapy]:::action ``` ### Why Other Options Are Suboptimal **MRI (Option B):** While GRE/SWI is excellent for detecting microhemorrhages and chronic blood products, it is **not** the first-line follow-up for acute ICH. MRI is time-consuming and less practical in the acute setting. It is useful later to assess underlying vascular lesions (AVM, cavernoma) in younger patients with lobar ICH. **CT Perfusion (Option C):** Useful for acute ischemic stroke to identify the ischemic penumbra, but **not standard** for ICH. It does not directly assess hematoma expansion. **Transcranial Doppler (Option D):** Used to detect vasospasm in SAH and to assess cerebral autoregulation, but not indicated in the acute phase of hypertensive ICH. **Tip:** Remember the **INTERACT-2 trial** (2013) — intensive BP lowering (target SBP < 140 mmHg) in acute ICH reduces hematoma expansion and improves outcomes. Repeat CT at 24 hours helps confirm whether this strategy is working. [cite:Harrison 21e Ch 297; Robbins 10e Ch 28] 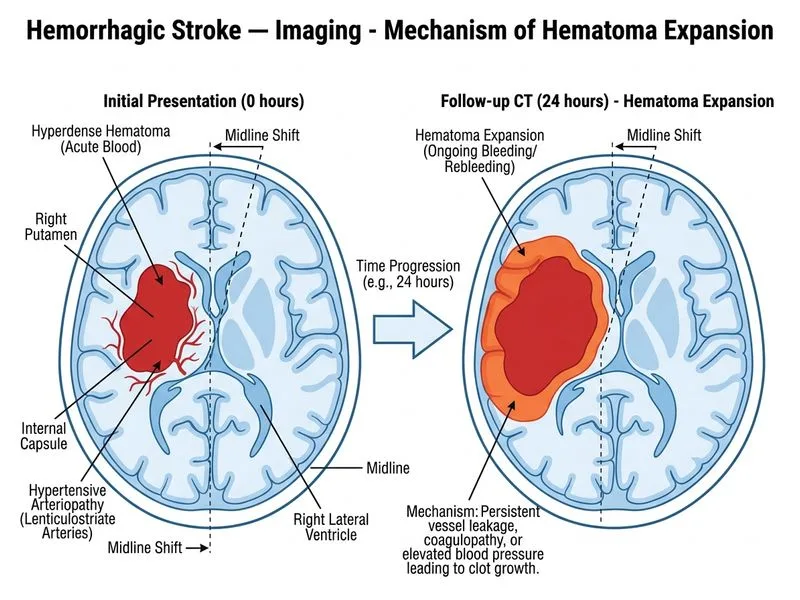
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.