## Clinical Scenario Analysis The patient presents with classic signs of **subarachnoid hemorrhage (SAH)**: sudden severe headache, meningeal signs (neck stiffness, photophobia), and CT confirmation of blood in the basal ganglia and ventricles. The next critical step is to identify the **source of bleeding** — typically a ruptured cerebral aneurysm in ~85% of non-traumatic SAH cases. ## Investigation Hierarchy for SAH Source Identification | Investigation | Role | Sensitivity for Aneurysm | Timing | Invasiveness | |---|---|---|---|---| | **CTA head/neck** | First-line screening | 95–98% | Immediate | Non-invasive | | **Digital subtraction angiography** | Gold standard; therapeutic capability | 100% | After CTA if positive | Invasive | | **MRI with gradient echo** | Detects blood; poor for aneurysm anatomy | ~70% | Slow; not acute | Non-invasive | | **Transcranial Doppler** | Monitors vasospasm; not diagnostic | N/A | Bedside | Non-invasive | ## Why Digital Subtraction Angiography is Correct **Key Point:** Digital subtraction cerebral angiography is the **gold standard** for definitive diagnosis and localization of cerebral aneurysms in SAH. It provides: - Highest spatial resolution and anatomical detail - Identification of aneurysm location, size, morphology, and neck - Assessment of parent vessel and collateral circulation - **Therapeutic capability**: allows endovascular coiling in the same procedure **Clinical Pearl:** In modern practice, **CTA is the first-line screening test** due to speed and non-invasiveness (95–98% sensitivity). However, the question asks for the investigation to **confirm diagnosis and identify source** — this is the specific role of **digital subtraction angiography**, which is both diagnostic and therapeutic. **High-Yield:** SAH management algorithm: 1. Non-contrast CT → confirms blood 2. CTA → screens for aneurysm (if available and high suspicion) 3. Digital subtraction angiography → **definitive diagnosis + intervention** If CTA is negative but clinical suspicion remains high, **lumbar puncture** (to detect xanthochromia) followed by angiography is indicated. 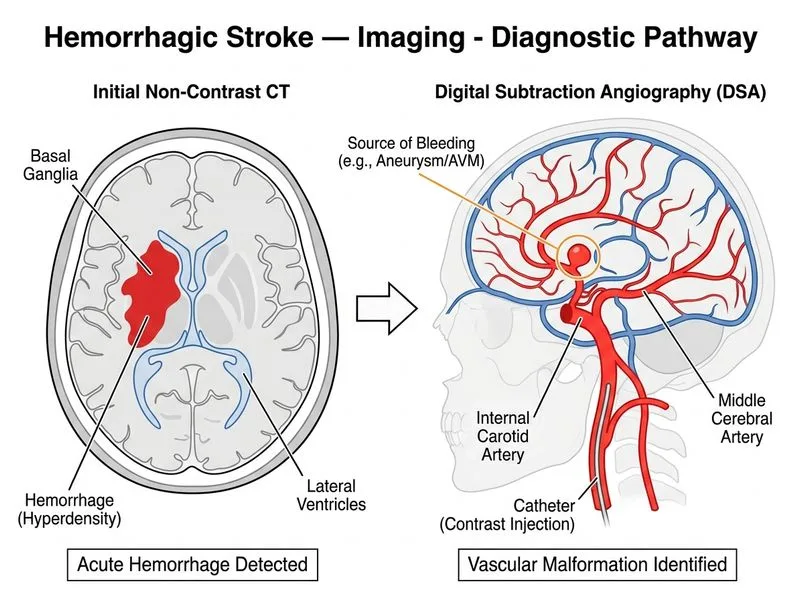
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.