## Clinical Scenario Analysis This patient presents with: - Severe thrombocytopenia (8,000/μL) - Mucocutaneous bleeding (gums, epistaxis, petechiae) - **Normal coagulation studies** (PT, aPTT, fibrinogen) - **Absence of schistocytes** (rules out TTP/HUS) - Acute onset (2 days) The normal coagulation profile and absence of hemolytic markers exclude DIC, TTP, and HUS. The clinical picture is **Immune Thrombocytopenia (ITP)**. ## Management Algorithm ```mermaid flowchart TD A[Severe thrombocytopenia<br/>+ mucocutaneous bleeding]:::outcome A --> B{Coagulation normal?<br/>No schistocytes?}:::decision B -->|Yes| C[Likely ITP]:::outcome C --> D{Bleeding symptoms?}:::decision D -->|Yes| E[Immediate platelet transfusion]:::action E --> F[Start corticosteroids<br/>prednisolone 1 mg/kg/day]:::action F --> G[Response in 3-7 days]:::outcome D -->|No| H[Observation ±<br/>corticosteroids]:::action ``` ## Why This Answer Is Correct **Key Point:** In acute ITP with **active bleeding**, the immediate management is **dual therapy**: platelet transfusion (for hemostasis) + corticosteroids (for immune modulation). **Clinical Pearl:** Platelet transfusion in ITP is **not contraindicated** when there is active bleeding; the transfused platelets may survive long enough to achieve hemostasis while steroids take effect (3–7 days). **High-Yield:** The sequence is: 1. **Platelet transfusion** → immediate hemostatic effect 2. **Corticosteroids** → reduce anti-platelet antibody production (onset 3–7 days) 3. Repeat transfusion if needed while awaiting steroid response ## Why Other Options Are Wrong | Option | Why Incorrect | |--------|---------------| | IVIG alone | IVIG (2 g/kg) is effective but slower (24–72 hrs) and is **second-line** when steroids fail or are contraindicated. In **active bleeding**, platelet transfusion + steroids is the standard first-line approach. | | Bone marrow biopsy | The clinical picture is classic for ITP (immune-mediated, not marrow failure). Biopsy is indicated only if diagnosis is unclear or to exclude aplasia—not in this acute presentation with normal coagulation. | | Defer treatment for anti-platelet antibodies | **Dangerous delay.** Anti-platelet antibody testing is a research tool and not routinely used to guide acute ITP management. Active bleeding requires **immediate intervention**, not waiting for serology. | ## Prognosis & Follow-Up **Key Point:** ~80% of acute ITP in adults respond to corticosteroids within 1–2 weeks. Platelet count recovery typically begins within 3–7 days. **Mnemonic:** **IVIG-STEROIDS-SPLENECTOMY** (IS-S) = the escalation ladder for ITP: - **I**IVIG or **S**teroids (first-line, depending on bleeding severity) - **S**plenectomy (second-line for steroid-dependent or refractory cases) **Warning:** Do not confuse ITP with TTP—in TTP, thrombocytopenia is accompanied by **schistocytes, hemolytic anemia, fever, renal dysfunction, and neurological symptoms**. TTP requires **plasma exchange**, not steroids or transfusion. 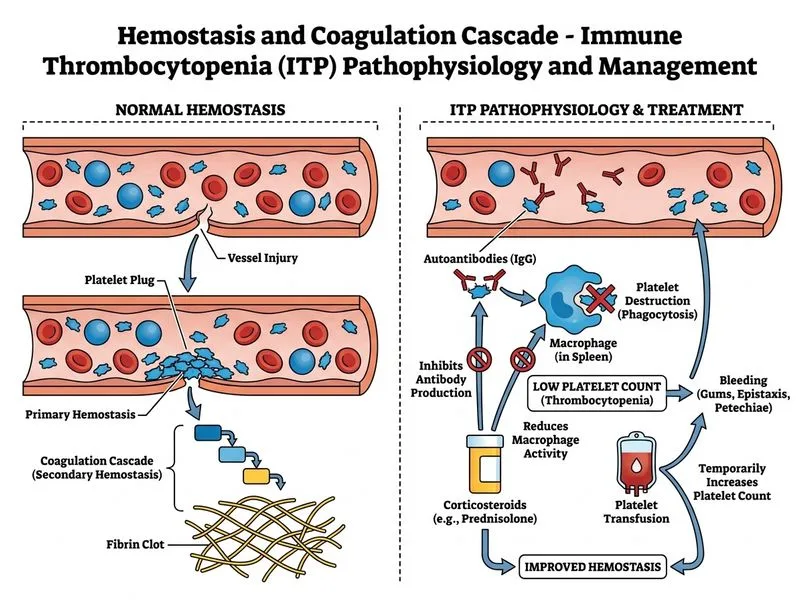
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.