## Clinical Diagnosis: Immune Thrombocytopenic Purpura (ITP) ### Key Clinical Features **Key Point:** The combination of severe thrombocytopenia (<20,000/μL), prolonged bleeding time, normal PT/aPTT, and normal bone marrow megakaryocytes is pathognomonic for ITP. ### Coagulation Profile Interpretation | Parameter | Finding | Interpretation | |-----------|---------|----------------| | Platelet count | 8,000/μL | Severe thrombocytopenia | | PT | 12 sec (normal) | Extrinsic pathway intact | | aPTT | 32 sec (normal) | Intrinsic pathway intact | | Bleeding time | Prolonged | Platelet dysfunction/deficiency | | Bone marrow | Normal megakaryocytes | Rules out bone marrow failure | ### Pathophysiology of ITP 1. Autoimmune destruction of platelets by IgG antibodies against platelet surface antigens (GPIIb/IIIa, GPIb/IX) 2. Increased platelet destruction in the spleen (reticuloendothelial system) 3. Bone marrow attempts compensatory megakaryopoiesis but cannot keep pace with destruction 4. Results in isolated thrombocytopenia with normal coagulation cascade function **High-Yield:** ITP is a diagnosis of exclusion — other causes of thrombocytopenia (sepsis, drugs, SLE, antiphospholipid syndrome) must be ruled out first. ### Why Coagulation Factors Are Normal in ITP **Clinical Pearl:** Coagulation factors (II, V, VII, VIII, IX, X, XI, XII) are synthesized by the liver and are unaffected in ITP. Bleeding occurs due to platelet deficiency, not factor deficiency. This is why PT and aPTT remain normal. ### Bleeding Manifestations - **Mucocutaneous bleeding:** Gingival bleeding, epistaxis, menorrhagia (platelet-dependent) - **Petechiae and ecchymoses:** Spontaneous capillary bleeding due to lack of platelet "plugs" - **Risk of intracranial hemorrhage:** If platelets <10,000/μL **Mnemonic:** **THROMBOCYTOPENIA** — Think: **T**hrombus deficiency, **H**emorrhage mucosal, **R**etic response (bone marrow), **O**utcome depends on count, **M**egakaryocytes normal, **B**leeding time prolonged, **O**ther factors normal, **C**oagulation cascade intact, **Y**ellow marrow (not infiltrated), **T**reatment with steroids/IVIG, **O**utcomes variable, **P**latelet antibodies present, **E**xclude secondary causes, **N**ormal PT/aPTT, **I**solated thrombocytopenia, **A**utoimmune mechanism. ### Diagnostic Criteria for ITP 1. Isolated thrombocytopenia (<150,000/μL) 2. Normal PT/aPTT (coagulation cascade intact) 3. Normal bone marrow with adequate megakaryocytes 4. Absence of splenomegaly or lymphadenopathy 5. Exclusion of secondary causes (SLE, APS, drugs, infections) [cite:Robbins 10e Ch 13] 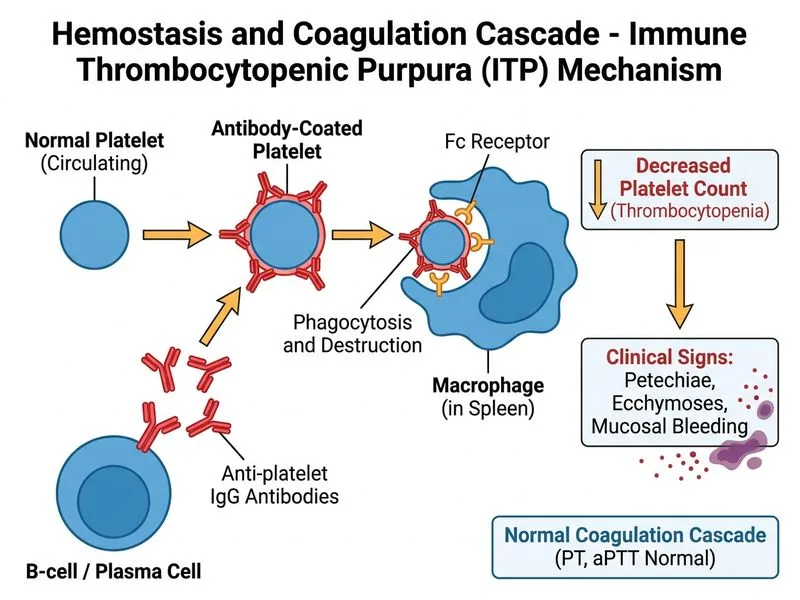
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.