## Diagnosis: Hepatocellular Carcinoma (HCC) ### Clinical Presentation This patient presents with the classic triad of HCC in a cirrhotic liver: 1. **Risk factors**: Alcohol-induced cirrhosis (20-year history) 2. **Symptoms**: Right upper quadrant pain, abdominal distension (ascites), jaundice 3. **Examination**: Hepatomegaly with hard, nodular surface (cirrhotic liver with tumor) ### Diagnostic Criteria (AASLD/EASL) **Key Point:** HCC diagnosis in cirrhotic patients is established by imaging criteria without need for biopsy when: - Lesion >1 cm with arterial phase hyperenhancement (APHE) + washout in portal venous or delayed phase on CT/MRI, OR - Lesion >1 cm with APHE on one imaging modality + elevated AFP (>400 ng/mL) **High-Yield:** This patient meets diagnostic criteria: - 4 cm lesion with arterial enhancement (APHE positive) - AFP 450 ng/mL (significantly elevated; >400 is highly specific for HCC) - Cirrhotic background (underlying liver disease) ### Serum AFP Interpretation | AFP Level | Clinical Significance | |-----------|----------------------| | <20 ng/mL | Normal | | 20–400 ng/mL | Nonspecific; can occur in cirrhosis, hepatitis | | >400 ng/mL | Highly suggestive of HCC (>90% specificity) | | >1000 ng/mL | Almost pathognomonic for HCC | **Clinical Pearl:** AFP is most useful as a diagnostic adjunct in cirrhotic patients with imaging findings; it is not a screening test alone due to low sensitivity in early HCC. ### Imaging Features of HCC **Arterial phase hyperenhancement (APHE)** is the hallmark: - Tumor receives blood supply predominantly from hepatic artery (unlike normal liver parenchyma) - Enhances early in arterial phase, then washes out in portal venous/delayed phases - This "arterial phase in, portal venous phase out" pattern is pathognomonic ### Why Cirrhosis Matters **Key Point:** Cirrhosis is the strongest risk factor for HCC development: - Alcohol-induced cirrhosis (as in this case) - Viral hepatitis (HBV, HCV) - NAFLD-related cirrhosis - Primary biliary cirrhosis - Hemochromatosis HCC arises in 1–5% of cirrhotic patients per year; surveillance with ultrasound ± AFP every 6 months is recommended. ### Pathological Features (if biopsy performed) - Trabecular, acinar, or solid growth pattern - Increased mitotic activity - Venous invasion (poor prognostic sign) - Capsule formation (common in HCC) [cite:Robbins 10e Ch 20] 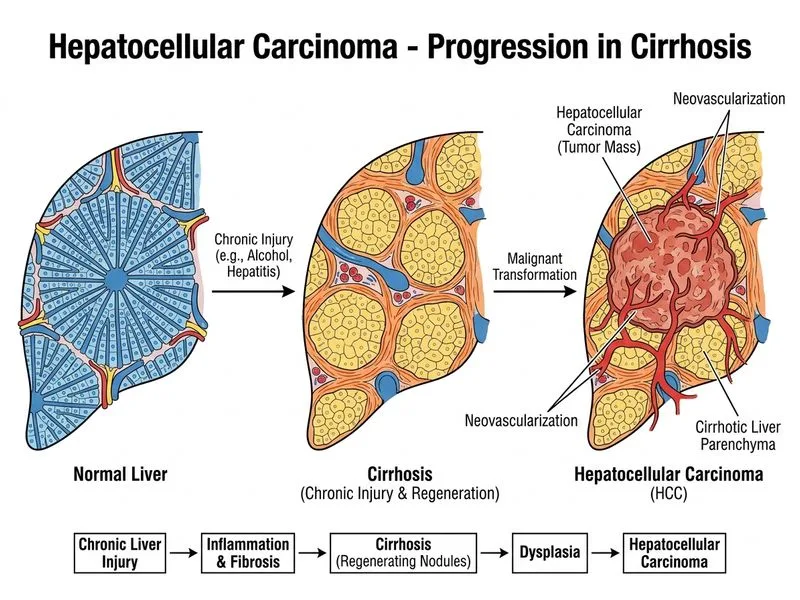
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.