## Diagnostic Dilemma: Nodule <2 cm in HBV Patient ### Clinical Context This patient has: - **Chronic HBV infection** (HBsAg+, HBeAg+) — major HCC risk factor - **No cirrhosis** (important: HCC can develop in non-cirrhotic HBV) - **Small nodule** (1.5 cm) with APHE but **no washout** - **Normal AFP** (35 ng/mL; <20–400 range) ### The Diagnostic Challenge **Key Point:** AASLD/EASL diagnostic criteria for HCC require: - **Lesion >1 cm**: APHE + washout on ONE imaging modality (CT or MRI), OR APHE on one modality + elevated AFP - **Lesion 1–2 cm**: Requires either (a) APHE + washout on both CT AND MRI, OR (b) biopsy confirmation - **Lesion <1 cm**: Surveillance; biopsy if high clinical suspicion **High-Yield:** This nodule is in the **1–2 cm "gray zone"** with APHE but **no washout**. It does not meet diagnostic criteria for definitive HCC on CT alone. ### Why Each Imaging Modality Matters | Modality | Strengths | Limitations | |----------|-----------|-------------| | **CT** | Fast, widely available, good for APHE detection | May miss washout in small lesions; metallic artifact | | **MRI** | Superior soft-tissue contrast, hepatobiliary agents (gadoxetate, gadobenate) enhance sensitivity for washout | Slower, contraindicated with certain implants | | **Ultrasound** | Real-time, no radiation, good for surveillance | Operator-dependent; limited in obese patients | **Clinical Pearl:** Hepatobiliary contrast agents (gadoxetate disodium, gadobenate dimeglumine) taken up by functioning hepatocytes cause delayed phase washout in HCC, improving diagnostic accuracy for small lesions. ### Management Algorithm for 1–2 cm Nodule ```mermaid flowchart TD A["Nodule 1-2 cm in HBV patient"]:::outcome --> B{"APHE on CT?"}:::decision B -->|"No"| C["Surveillance in 3 months"]:::action B -->|"Yes"| D{"Washout on CT?"}:::decision D -->|"Yes"| E["HCC diagnosed"]:::outcome D -->|"No"| F["Perform MRI with hepatobiliary contrast"]:::action F --> G{"APHE + washout on MRI?"}:::decision G -->|"Yes"| E G -->|"No"| H["Biopsy or close surveillance"]:::action ``` ### Why MRI is the Next Step **Key Point:** MRI with hepatobiliary contrast agents (gadoxetate) is the gold standard for characterizing 1–2 cm nodules because: 1. **Higher sensitivity for washout** in small lesions compared to CT 2. **Hepatobiliary agents** are taken up by normal hepatocytes but not by HCC cells → delayed phase washout is more pronounced 3. **Can establish definitive diagnosis** without biopsy if APHE + washout is confirmed 4. **No radiation exposure** (advantage over repeat CT) ### Why NOT the Other Options **Repeat imaging in 3 months** (Option A): - Delays diagnosis in a patient with HBV and a suspicious nodule - Appropriate only if initial imaging is completely benign; this nodule shows APHE (suspicious) **Immediate biopsy** (Option B): - Reserved for lesions that do NOT meet imaging criteria after comprehensive imaging - Biopsy carries risk (hemorrhage, seeding) and should be avoided if imaging can clarify diagnosis - MRI should be attempted first **Sorafenib therapy** (Option C): - Indicated only for **advanced HCC** (BCLC stage C) with extrahepatic spread or vascular invasion - This patient has a small, localized nodule; staging and confirmation of diagnosis must precede systemic therapy - Premature systemic therapy is inappropriate ### Prognostic Significance: HCC in Non-Cirrhotic HBV **Clinical Pearl:** HBV-related HCC can develop without cirrhosis, especially in patients with high viral load and active inflammation. These tumors may have: - Better prognosis if detected early (small size) - Potential for curative resection or ablation if confined to liver - Need for aggressive antiviral therapy (nucleos(t)ide analogues) to prevent recurrence [cite:Robbins 10e Ch 20; AASLD HCC Diagnosis Guidelines 2018] 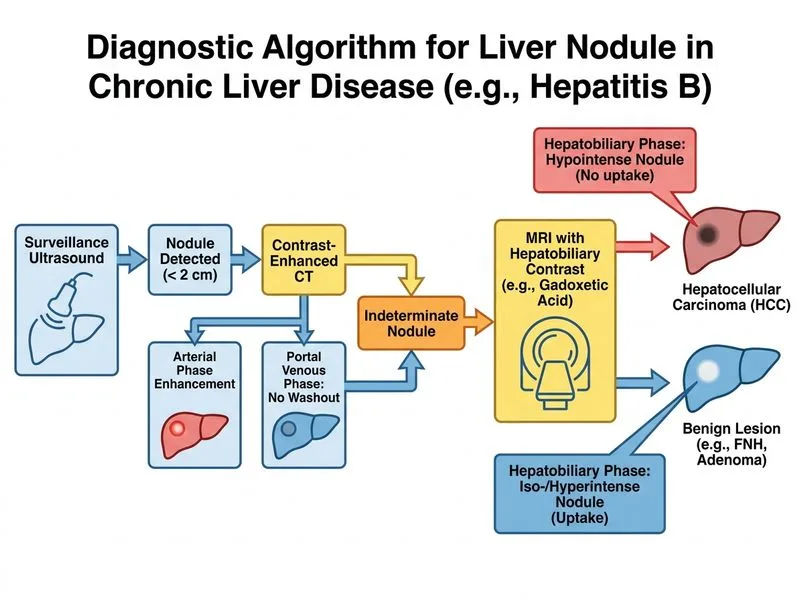
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.