## Clinical Diagnosis: Hepatocellular Carcinoma ### Key Clinical Features **Key Point:** The combination of cirrhotic liver disease (chronic HBV), markedly elevated AFP (>400 ng/mL is highly suggestive), and imaging findings of arterial hyperenhancement in a nodule >1 cm establishes HCC diagnosis without need for biopsy. ### Diagnostic Criteria (AASLD/EASL) For nodules in cirrhotic livers: | Nodule Size | Imaging Criteria for HCC Diagnosis | |---|---| | >2 cm | One imaging modality (CT/MRI/US) with arterial phase hyperenhancement (APHE) + washout | | 1–2 cm | Two imaging modalities showing APHE + washout, OR one imaging modality + AFP >400 ng/mL | | <1 cm | Surveillance; biopsy if high suspicion | **Clinical Pearl:** In this patient, the 4 cm mass with APHE on ultrasound + AFP 1200 ng/mL + cirrhotic liver (HBsAg+) meets diagnostic criteria for HCC without biopsy. ### Risk Factors Present 1. **Chronic hepatitis B** — most common cause of HCC in Asia-Pacific region 2. **Cirrhosis** — evident from clinical signs (jaundice, ascites, hard nodular hepatomegaly) 3. **Age >50** — typical presentation age ### Pathophysiology Chronic HBV infection → chronic inflammation → cirrhosis → dysplastic nodules → HCC. HBV integration into hepatocyte genome and HBx protein expression drive malignant transformation. **High-Yield:** AFP >400 ng/mL in a cirrhotic patient with a nodule is diagnostic for HCC; biopsy is unnecessary and may seed tumor. ### Imaging Hallmark **Arterial phase hyperenhancement (APHE)** followed by **venous/delayed phase washout** is the pathognomonic imaging signature of HCC — reflects tumor's arterial blood supply (from hepatic artery) rather than portal venous supply of normal liver parenchyma. 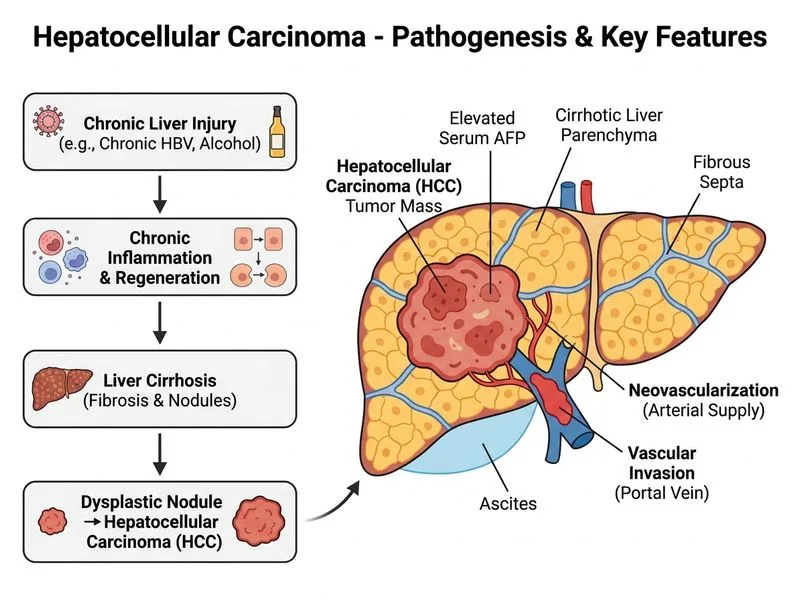
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.