## Investigation of Choice for HCC Confirmation and Staging ### Why MRI with Hepatobiliary Contrast is Superior **Key Point:** MRI with hepatobiliary contrast agents (gadoxetate, gadobenate) is the most specific imaging modality for: 1. **Diagnosis confirmation** — characteristic enhancement pattern (arterial enhancement + washout + hepatobiliary phase) 2. **Vascular invasion assessment** — superior soft tissue contrast resolution 3. **Tumor staging** — detects satellite nodules, intrahepatic metastases 4. **Diffusion-weighted imaging (DWI)** — high b-values improve lesion conspicuity and characterization ### Comparison of Imaging Modalities for HCC | Modality | Sensitivity | Specificity | Vascular Invasion Detection | Hepatobiliary Phase | |---|---|---|---|---| | **CT (triphasic)** | 80–90% | 85–95% | Moderate | No | | **MRI (hepatobiliary)** | 90–95% | 95–98% | **Excellent** | **Yes** | | **Ultrasound** | 60–80% | 70–85% | Poor | No | | **PET-FDG** | 50–70% | 60–75% | Poor | No | **High-Yield:** MRI is particularly superior for: - Small nodules (<2 cm) - Cirrhotic livers with background fibrosis - Detection of portal vein thrombosis (vascular invasion) - Hepatobiliary phase washout (HCC does not take up hepatobiliary contrast) ### Clinical Pearl In a patient with markedly elevated AFP (>1200 ng/mL) and cirrhosis, MRI provides the **highest specificity** for confirming HCC and staging vascular invasion — critical for treatment planning (TACE, sorafenib, surgical resection eligibility). ### Why DWI Matters Diffusion-weighted imaging increases HCC detection by showing restricted diffusion (high cellularity), distinguishing HCC from benign cirrhotic nodules. [cite:Robbins 10e Ch 18; Harrison 21e Ch 297] 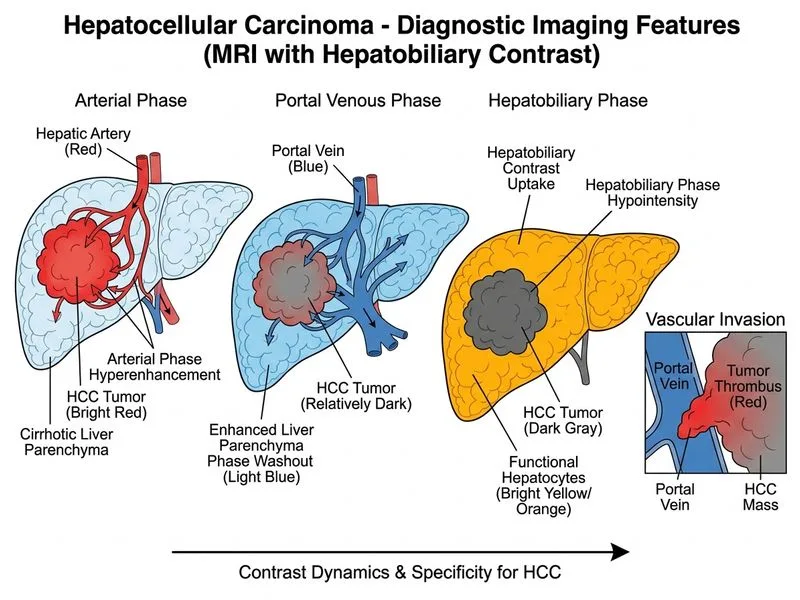
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.