## Clinical Presentation Analysis This patient presents with classic **herpes zoster (shingles)** in an immunocompetent host: - Dermatomal distribution (T5 dermatome) - Vesicles on erythematous base - Severe pain and burning (neuropathic) - Early presentation (3 days — within the treatment window) ## Management Strategy ### Key Point: **Antiviral therapy must be initiated within 72 hours of rash onset** to reduce duration of acute pain, prevent dissemination, and reduce post-herpetic neuralgia (PHN) risk. ### High-Yield: In **immunocompetent patients with localized zoster**, oral acyclovir 800 mg five times daily for 7–10 days is the standard first-line agent. This dose is specifically chosen for zoster (higher than for HSV). ## Dosing Regimen | Agent | Dose (Immunocompetent) | Duration | Notes | |-------|------------------------|----------|-------| | **Acyclovir (oral)** | 800 mg 5× daily | 7–10 days | First-line; requires frequent dosing | | **Valacyclovir (oral)** | 1000 mg 3× daily | 7 days | Better bioavailability; preferred if available | | **Famciclovir (oral)** | 500 mg 3× daily | 7 days | Longest intracellular half-life | ### Clinical Pearl: Early antiviral therapy (within 72 hours) reduces: - Duration of acute pain by ~1 week - Incidence of PHN in patients >50 years by ~50% - Risk of dissemination and visceral involvement ## Adjunctive Management 1. **Analgesics**: Paracetamol, NSAIDs, or gabapentin for neuropathic pain 2. **Topical care**: Calamine lotion, cool compresses (do NOT use occlusive dressings) 3. **Secondary infection prevention**: Keep lesions clean and dry ### Warning: Do NOT delay antiviral therapy awaiting confirmatory testing in a clinically obvious case — the 72-hour window is critical. 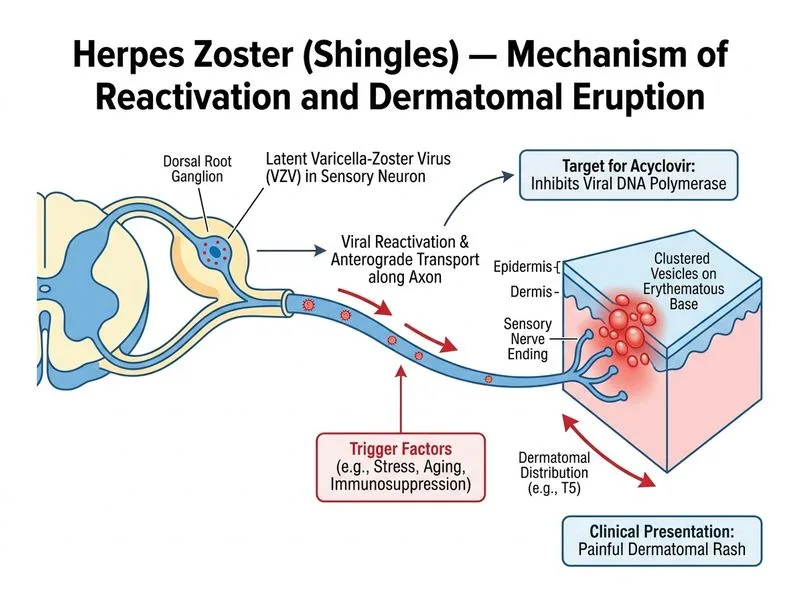
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.