## Diagnosis: Posterior Hip Dislocation ### Clinical Presentation The classic triad of **posterior hip dislocation** is: 1. **Flexion, adduction, and internal rotation (FAIR) posture** — the hip is "locked" in this position 2. **Apparent shortening** of the affected limb (flexion causes relative shortening) 3. **Severe pain** on any movement, especially attempts at external rotation or abduction **Key Point:** Posterior dislocation accounts for 80–90% of hip dislocations and is classically associated with **flexed knee + flexed hip** (dashboard injury, high-energy trauma). ### Anatomical Basis of the FAIR Posture ```mermaid flowchart TD A[Posterior Hip Dislocation]:::outcome --> B[Femoral head displaced posteriorly]:::outcome B --> C{Capsular stretch?}:::decision C -->|Yes| D[MFCA stretched posteriorly]:::urgent C -->|Yes| E[Capsule under tension]:::urgent D --> F[Pain from vascular compromise]:::outcome E --> F F --> G[Protective FAIR posture adopted]:::action G --> H[Flexion + adduction + IR<br/>relieves capsular tension]:::action H --> I[Pain reduced, muscle spasm minimized]:::outcome ``` ### Why FAIR Relieves Pain | Movement | Effect on Posterior Capsule | Effect on MFCA | |----------|----------------------------|----------------| | Flexion | Relaxes posterior capsule | Reduces stretch | | Adduction | Brings femoral head medially | Reduces posterior displacement | | Internal rotation | Internally rotates femur | Reduces external rotator tension | **Clinical Pearl:** The **medial femoral circumflex artery (MFCA)** enters the hip joint via the posterior capsule. In posterior dislocation, the femoral head is displaced posteriorly, stretching the MFCA and posterior capsule. The FAIR posture is a protective reflex that minimizes this stretch and reduces pain. ### Distinguishing Features: Posterior vs. Anterior Dislocation | Feature | Posterior Dislocation | Anterior Dislocation | |---------|----------------------|---------------------| | Hip position | Flexion, adduction, IR | Flexion, abduction, ER | | Apparent length | Shortened | Lengthened | | Mechanism | Flexed knee + flexed hip (dashboard) | Forced abduction + ER | | Frequency | 80–90% | 10–20% | | Sciatic nerve injury | 10–15% | Rare | **High-Yield:** Always check for **sciatic nerve injury** (foot drop, sensory loss in S1 distribution) in posterior dislocation — it is the most common neurological complication. ### Management 1. **Immediate:** Neurovascular assessment (this patient has intact pulses and sensation — good prognostic sign) 2. **Reduction:** Closed reduction under anesthesia (Allis maneuver for posterior dislocation) 3. **Imaging:** Post-reduction CT to rule out associated acetabular or femoral head fractures 4. **Follow-up:** Monitor for late complications (avascular necrosis of femoral head, post-traumatic arthritis) **Warning:** Delay in reduction >12 hours significantly increases risk of AVN due to prolonged vascular compromise. 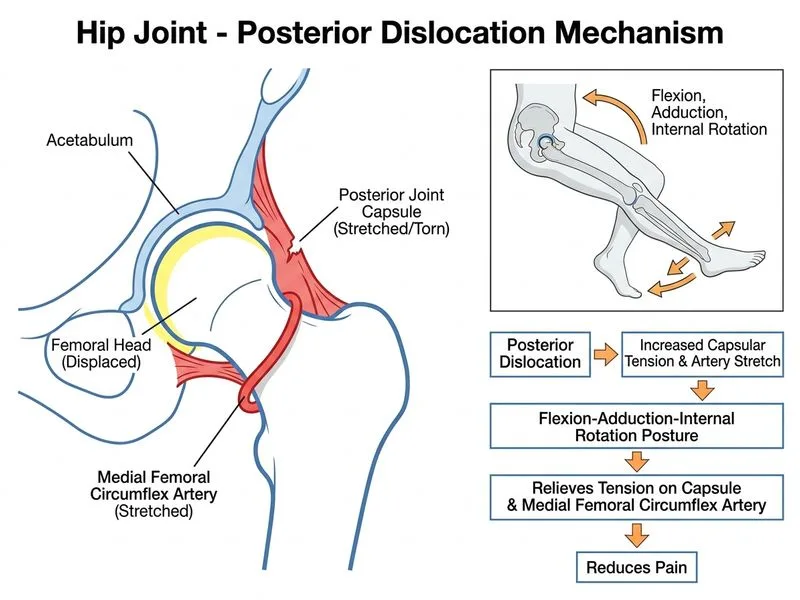
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.