## Clinical and Radiological Correlation The clinical scenario and HRCT findings in this case are most consistent with **Acute Exacerbation of COPD with Superimposed Bacterial Pneumonia** (Option D). ### Key Clinical Features **High-Yield:** This patient has a **20-year history of COPD** — not IPF or any interstitial lung disease. The acute presentation with worsening dyspnea and hemoptysis, combined with focal consolidation with air bronchograms in the right upper lobe, is the classic picture of bacterial pneumonia complicating COPD. ### Interpreting the HRCT Findings 1. **Consolidation with air bronchograms (right upper lobe)** — hallmark of acute bacterial pneumonia (lobar/segmental consolidation with patent airways) 2. **Irregular linear opacities and traction bronchiectasis (bilateral lower lobes)** — chronic architectural distortion from long-standing COPD; peribronchial fibrosis and airway remodeling are well-recognized sequelae of severe COPD 3. **No mention of honeycombing** — the absence of honeycombing argues strongly against UIP/IPF pattern 4. **No diffuse ground-glass opacification** — argues against AIP (diffuse alveolar damage) or NSIP ### Why NOT UIP Pattern (Option A)? **Key Point:** UIP pattern requires **honeycombing** (with or without traction bronchiectasis) in a **subpleural, basal-predominant** distribution, as defined by the Fleischner Society and ATS/ERS/JRS/ALAT guidelines. The stem describes traction bronchiectasis and linear opacities but **no honeycombing**, and the patient's primary diagnosis is COPD — not IPF. Attributing these findings to UIP in a known COPD patient without a prior ILD diagnosis is diagnostically unsound. ### Why NOT AIP (Option B)? AIP presents with **diffuse bilateral ground-glass opacification** and consolidation (diffuse alveolar damage pattern), typically in a previously healthy individual with rapid progression to respiratory failure. The focal right upper lobe consolidation and chronic lower lobe changes do not fit AIP. ### Why NOT NSIP (Option C)? NSIP shows **bilateral, symmetric ground-glass opacification** with lower lobe predominance and subpleural sparing. It is associated with connective tissue diseases, not COPD. Acute decompensation of NSIP would not produce focal lobar consolidation. ### Differential Summary | Feature | COPD + Pneumonia | UIP + Infection | AIP | NSIP | |---------|-----------------|-----------------|-----|------| | **Background history** | COPD (20 years) | IPF/ILD | None (acute) | CTD/idiopathic | | **Honeycombing** | Absent | Present | Absent | Absent | | **Consolidation pattern** | Focal (lobar) | Patchy | Diffuse bilateral | Rare | | **Air bronchograms** | Present | Present | Present | May be present | | **Traction bronchiectasis** | Can occur in COPD | Prominent | Absent | Mild | **Clinical Pearl:** In a patient with known COPD, new focal consolidation with air bronchograms = bacterial pneumonia until proven otherwise. Chronic lower lobe linear opacities and traction bronchiectasis in COPD reflect peribronchial fibrosis and airway remodeling — they do NOT establish a diagnosis of UIP/IPF in the absence of honeycombing and a clinical ILD history. [cite: Harrison's Principles of Internal Medicine 21e, Ch. 285 (COPD) & Ch. 297 (ILD); Fleischner Society HRCT Glossary 2014] 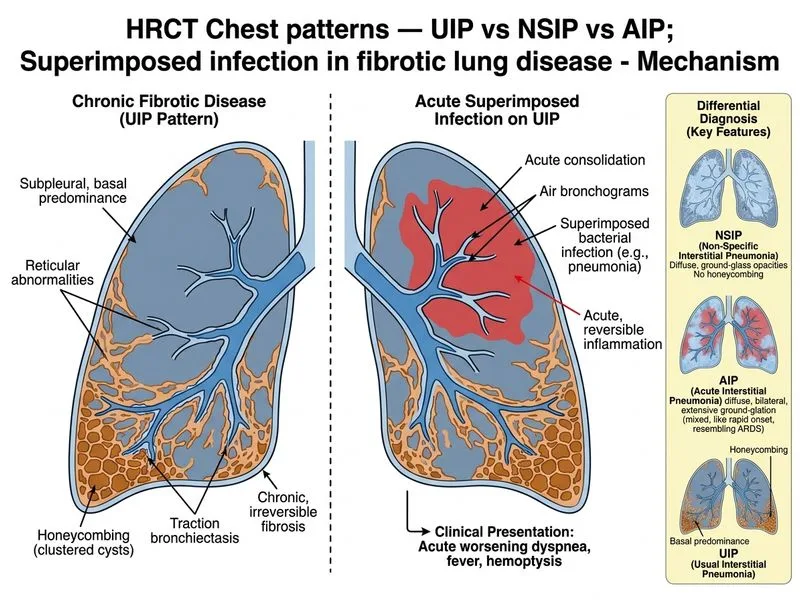
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.