## Assessment of Hypertensive Retinopathy Severity ### Clinical Context This patient presents with signs of **acute hypertensive retinopathy** (flame hemorrhages, cotton-wool spots, hard exudates, disc edema), indicating end-organ damage requiring urgent evaluation and management. ### Role of OCT in Hypertensive Retinopathy **Key Point:** OCT is the investigation of choice for assessing structural changes in hypertensive retinopathy, particularly macular and optic disc involvement. ### What OCT Demonstrates | Finding | Clinical Significance | |---------|----------------------| | Macular thickening/edema | Indicates hypertensive macular edema (HME) | | Disrupted ellipsoid zone | Photoreceptor damage; prognostic indicator | | Optic disc edema quantification | Severity assessment; guides BP control urgency | | Retinal fold patterns (Paton's lines) | Chronic hypertensive changes | | Choroidal thickening | Acute hypertensive response | ### Why OCT is Superior for This Case 1. **Non-invasive & rapid** — no dye injection needed in acute setting 2. **Quantifies macular edema** — critical for determining visual prognosis 3. **Assesses optic disc edema** — objective measure of severity 4. **Guides follow-up** — baseline for monitoring response to antihypertensive therapy 5. **No contraindications** — safe even with renal impairment (common in hypertensive patients) **High-Yield:** OCT has largely replaced FFA as the first-line imaging in hypertensive retinopathy because it provides structural detail without systemic dye load and is superior for quantifying macular involvement. **Clinical Pearl:** The presence of **macular edema with disrupted ellipsoid zone** on OCT indicates more severe retinal damage and warrants aggressive BP control to prevent permanent vision loss. ### Keith-Wagener-Barker Classification Context OCT helps objectively grade severity: - **Grade III:** Retinal hemorrhages, exudates, cotton-wool spots → OCT shows macular thickening - **Grade IV:** Optic disc edema + all Grade III findings → OCT quantifies disc edema and macular involvement [cite:Parson's Diseases of the Eye 22e Ch 12] 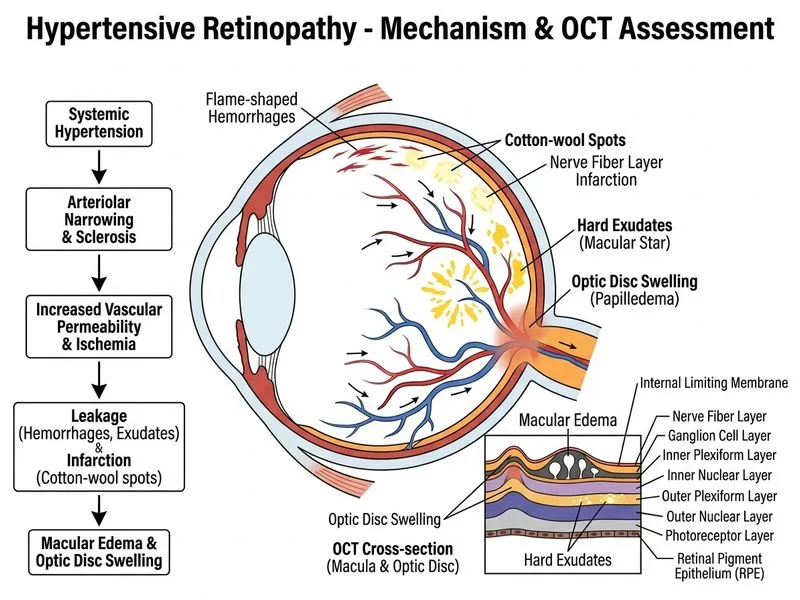
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.