## Investigation for Ischemic Assessment in Hypertensive Retinopathy ### Clinical Context This patient has **chronic hypertensive retinopathy (Grade III)** without acute symptoms. The goal is to: - Detect **capillary nonperfusion** and ischemic areas - Assess risk of progression to malignant hypertension - Guide intensity of blood pressure control ### Why FFA is Correct **Key Point:** Fundus fluorescein angiography (FFA) is the gold standard for detecting ischemic changes in hypertensive retinopathy because it: - Visualizes **capillary nonperfusion** areas (dark zones without fluorescence) - Identifies **cotton-wool spot** perfusion defects - Detects **microaneurysms** and retinal ischemia - Reveals **neovascularization** (sign of severe ischemia) - Assesses **retinal perfusion pressure** and vascular competence **High-Yield:** FFA findings that indicate **high risk of progression**: - Extensive capillary nonperfusion (>5 disc areas) - Retinal arteriolar narrowing with delayed arteriovenous transit time - Presence of microaneurysms - Breakdown of blood-retinal barrier (retinal edema) ### When FFA is Indicated in Hypertensive Retinopathy | Clinical Scenario | FFA Role | |---|---| | **Chronic Grade III retinopathy** (asymptomatic) | Assess ischemia burden and risk stratification — **THIS CASE** | | **Suspected malignant hypertension** | Confirm ischemic retinopathy; guide urgent BP control | | **Vision loss with hemorrhages/exudates** | Differentiate ischemic vs. edema-related vision loss | | **Neovascularization suspected** | Confirm and map areas of nonperfusion driving NV | | **Monitoring response to treatment** | Serial FFA to assess reperfusion | ### Why Other Investigations Are Suboptimal **OCT of Optic Nerve Head:** - Shows structural changes (disc swelling, RNFL thinning) but does NOT assess perfusion - Useful for detecting optic disc edema but not ischemia - Does not guide risk stratification for ischemic progression **Automated Perimetry:** - Detects functional loss (scotomas) but is a **late finding** - Not sensitive for early ischemia - Visual fields may be normal in early-to-moderate hypertensive retinopathy - Better suited for glaucoma or advanced ischemic retinopathy **Indocyanine Green Angiography (ICGA):** - Visualizes **choroidal circulation** (not retinal) - Used for choroidal neovascularization, polypoidal choroidal vasculopathy - Not indicated for assessing retinal ischemia in hypertensive retinopathy - Inferior to FFA for retinal perfusion assessment ### Diagnostic Algorithm: Hypertensive Retinopathy Risk Stratification ```mermaid flowchart TD A[Hypertensive Retinopathy Grade III]:::outcome --> B{Symptoms or Vision Loss?}:::decision B -->|Yes| C[Perform OCT Macula]:::action C --> D[Assess Macular Edema]:::action B -->|No| E[Perform FFA]:::action E --> F[Assess Capillary Nonperfusion]:::action F --> G{Extensive Nonperfusion?}:::decision G -->|Yes| H[High Risk of Progression]:::urgent G -->|No| I[Low-Moderate Risk]:::outcome H --> J[Aggressive BP Control + Close Follow-up]:::action I --> K[Standard BP Control + Annual FFA]:::action ``` **Clinical Pearl:** **Capillary nonperfusion >5 disc areas** on FFA is a strong predictor of progression to malignant hypertensive retinopathy within 1–2 years and warrants intensification of antihypertensive therapy. **Mnemonic: FFA in Hypertensive Retinopathy — "ISCHEMIA"** - **I** — Ischemic areas (nonperfusion) - **S** — Structural changes (microaneurysms, hemorrhages) - **C** — Capillary integrity assessment - **H** — Hemodynamic evaluation (AV transit time) - **E** — Edema quantification (retinal thickening) - **M** — Microaneurysms detection - **I** — Ischemic risk stratification - **A** — Assess neovascularization risk [cite:Harrison 21e Ch 29; Park 26e Ch 10] 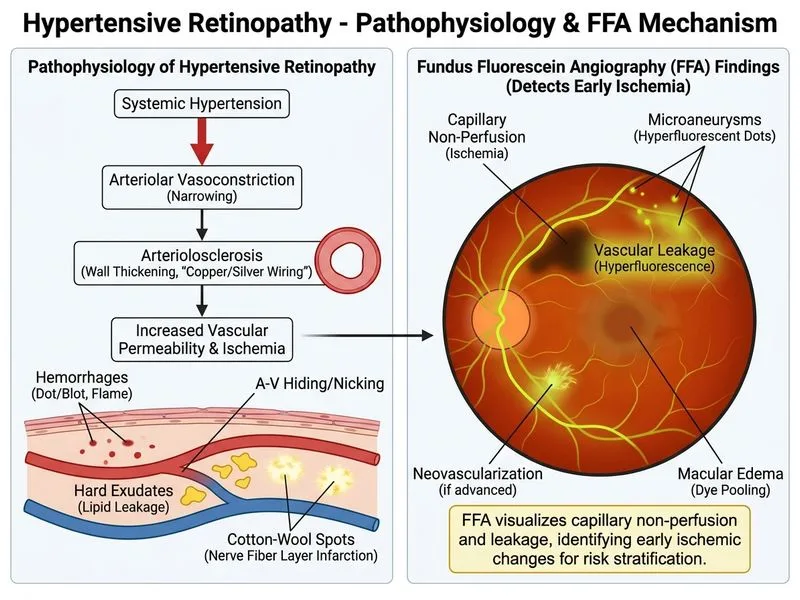
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.