## Clinical Presentation Analysis This patient presents with **hypertensive retinopathy with papilledema**, indicating **hypertensive emergency** (also called malignant hypertension). The constellation of findings—flame hemorrhages, cotton-wool spots, hard exudates in a macular star pattern, and papilledema—represents Grade IV hypertensive retinopathy. **Key Point:** Papilledema in the setting of hypertension is a hallmark of hypertensive emergency and mandates immediate, aggressive BP reduction to prevent irreversible end-organ damage (retina, kidney, brain). ## Management Algorithm for Hypertensive Emergency ```mermaid flowchart TD A[Hypertensive Emergency<br/>BP > 180/120 + end-organ damage]:::outcome --> B{Papilledema or<br/>acute vision loss?}:::decision B -->|Yes| C[Admit ICU/HDU]:::action C --> D[IV antihypertensive agents]:::action D --> E[Target: 25% BP reduction<br/>in first 1 hour]:::action E --> F[Then gradual reduction<br/>to goal over 24 hrs]:::action F --> G[Fundoscopy + labs<br/>to monitor response]:::outcome B -->|No| H[Oral agents<br/>Outpatient follow-up]:::action ``` ## Why Immediate IV Therapy? **High-Yield:** Hypertensive emergency with retinal signs (papilledema, hemorrhage, exudates) requires **inpatient admission and IV antihypertensive therapy**. The goal is to reduce mean arterial pressure by **25% in the first hour**, then cautiously to target over 24 hours. Overly rapid reduction risks stroke; too slow risks progressive retinal/renal damage. **Clinical Pearl:** The presence of papilledema distinguishes this from chronic hypertensive retinopathy (Grade III) and mandates emergent intervention. Papilledema indicates elevated intracranial pressure from hypertensive encephalopathy. **Warning:** Do NOT reduce BP by >25% in the first hour or to normal range acutely—this can precipitate stroke due to loss of cerebral autoregulation in chronically hypertensive patients. ## Appropriate Agents for IV Therapy | Agent | Onset | Duration | Use Case | |-------|-------|----------|----------| | Labetalol | 5–10 min | 3–6 hrs | First-line for most hypertensive emergencies | | Nicardipine | 5–10 min | 15–30 min | Preferred in renal disease | | Esmolol | 1–2 min | 10–20 min | Acute MI, tachycardia | | Hydralazine | 10–20 min | 4–6 hrs | Pregnancy-related hypertension | | Sodium nitroprusside | Immediate | 1–3 min | Refractory cases (ICU only) | **Key Point:** Fundoscopy and basic labs (electrolytes, creatinine, urinalysis) should be obtained after admission to assess baseline end-organ involvement, but these do NOT delay initiation of IV therapy. 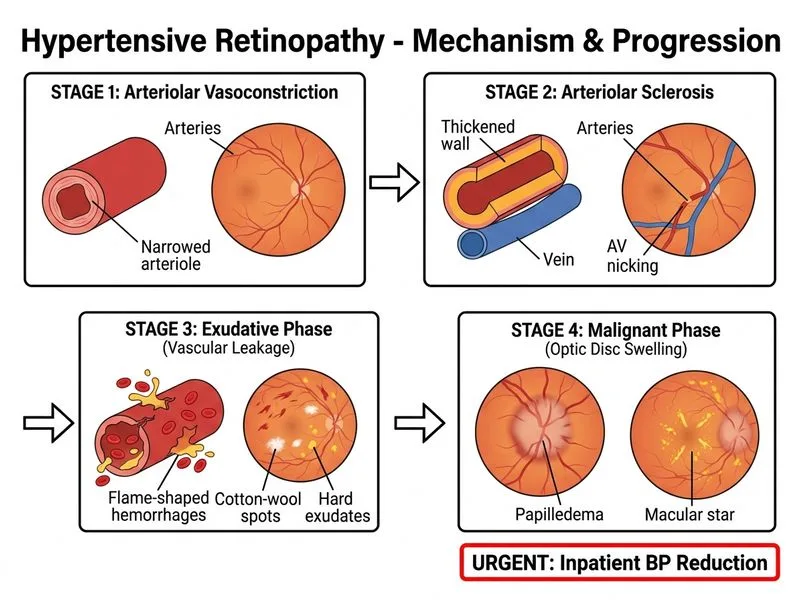
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.