## Clinical Presentation Analysis This patient has **Grade III hypertensive retinopathy** (microaneurysms, dot-blot hemorrhages, hard exudates, NO papilledema) with **preserved visual acuity**. This is **hypertensive retinopathy without hypertensive emergency**—a chronic manifestation requiring systemic BP control rather than acute IV therapy. **Key Point:** The absence of papilledema and preserved vision indicate this is NOT hypertensive emergency. Management focuses on optimizing systemic antihypertensive therapy and monitoring for progression. ## Grading of Hypertensive Retinopathy | Grade | Findings | Papilledema | Management | |-------|----------|-------------|-------------| | I | Arteriolar narrowing, AV nicking | No | Optimize BP control | | II | Grade I + microaneurysms, dot hemorrhages | No | Optimize BP control | | III | Grade II + hard exudates, cotton-wool spots | No | Optimize BP control + monitor | | IV | Grade III + papilledema | **Yes** | **Hypertensive emergency: IV therapy** | **High-Yield:** The presence or absence of **papilledema** is the critical discriminator between chronic hypertensive retinopathy (Grades I–III) and hypertensive emergency (Grade IV). Papilledema = emergency; no papilledema = chronic management. ## Management Strategy for Grade III Hypertensive Retinopathy ```mermaid flowchart TD A[Grade III Hypertensive Retinopathy<br/>No papilledema, VA preserved]:::outcome --> B[Optimize systemic BP control]:::action B --> C[Target BP < 140/90 mmHg]:::action C --> D[Repeat fundoscopy in 3-6 months]:::action D --> E{Progression or<br/>vision loss?}:::decision E -->|Yes| F[Consider FFA + laser]:::action E -->|No| G[Continue monitoring]:::action G --> H[Annual fundoscopy]:::action ``` **Clinical Pearl:** Hypertensive retinopathy is **reversible** if BP is controlled early. Hard exudates may persist but hemorrhages and microaneurysms typically resolve with adequate antihypertensive therapy over weeks to months. **Warning:** Do NOT mistake Grade III hypertensive retinopathy for diabetic retinopathy. While both show microaneurysms and hard exudates, the clinical context (hypertension vs. diabetes), absence of venous beading, and response to BP control help differentiate. ## Role of Fundus Fluorescein Angiography (FFA) FFA is **not routinely indicated** at this stage because: - Visual acuity is preserved (6/9) - No macular edema is clinically apparent - FFA is reserved for cases with **vision-threatening macular involvement** or to assess retinal perfusion if progression occurs If the patient develops vision loss or FFA shows macular ischemia, then laser photocoagulation may be considered. 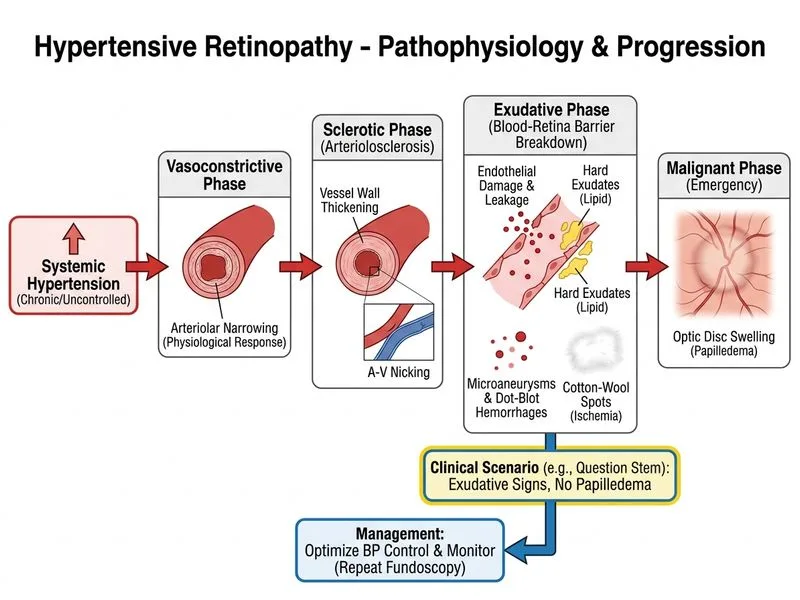
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.