## Management of Non-bullous Impetigo: First-Line Therapy ### Clinical Context **Key Point:** The clinical presentation—thick, adherent crusts; progression from papule → pustule → crust; and localized distribution—is classic for non-bullous impetigo. The β-lactamase–producing *S. aureus* isolate rules out penicillin-based monotherapy. **High-Yield:** For localized impetigo (< 5 lesions or limited body surface area), **topical antibiotics are first-line**. Mupirocin is the gold standard topical agent for impetigo. ### Why Mupirocin Is the Correct Choice 1. **Mechanism of action:** Mupirocin inhibits bacterial isoleucyl-tRNA synthetase, preventing protein synthesis. It is bactericidal against *S. aureus* and *S. pyogenes*. 2. **Efficacy:** Cure rates of 85–95% for non-bullous impetigo when applied topically. 3. **Guideline recommendation:** WHO, AAD, and Indian Academy of Dermatology recommend topical mupirocin as first-line for localized impetigo. 4. **Resistance:** Mupirocin resistance in *S. aureus* remains low (< 5% globally). 5. **Advantages:** Minimal systemic absorption, low risk of adverse effects, cost-effective, and prevents spread. ### Impetigo Management Algorithm ```mermaid flowchart TD A[Non-bullous Impetigo Diagnosis]:::outcome --> B{Extent of Disease?}:::decision B -->|Localized: < 5 lesions or < 2% BSA| C[Topical Mupirocin]:::action B -->|Extensive: > 5 lesions or > 2% BSA| D[Systemic Antibiotic]:::action B -->|Bullous or Systemic Signs| E[Systemic Antibiotic]:::action C --> F[Apply TID for 7–10 days]:::action D --> G{β-lactamase Producer?}:::decision E --> G G -->|Yes| H[Cephalosporin or Fluoroquinolone]:::action G -->|No| I[Amoxicillin or Penicillin V]:::action H --> J[Review at 48 hrs]:::decision I --> J J -->|Improved| K[Continue to cure]:::outcome J -->|No improvement| L[Switch to alternative]:::urgent ``` ### Why Other Options Are Incorrect | Option | Why It Is Wrong | |--------|----------------| | **Amoxicillin** | β-lactamase–producing *S. aureus* will hydrolyze amoxicillin, rendering it ineffective. This is a trap answer for students who forget the resistance mechanism. | | **Cefazolin** | While cefazolin is a valid systemic option for extensive impetigo, it is NOT first-line for localized disease. Topical therapy is preferred to minimize systemic exposure and cost. | | **Clindamycin** | Clindamycin is a reasonable alternative for MRSA impetigo, but it is NOT first-line. Mupirocin topical is preferred for localized disease. Clindamycin is reserved for systemic or extensive impetigo. | **Clinical Pearl:** The presence of regional lymphadenopathy (lymphangitis) does NOT mandate systemic therapy if the skin lesions are localized and the child is systemically well. Topical mupirocin with close follow-up is still appropriate. **Warning:** Do not confuse "β-lactamase–producing" with "MRSA." β-lactamase–producing *S. aureus* is typically methicillin-susceptible and will respond to cephalosporins or fluoroquinolones. True MRSA requires clindamycin, fluoroquinolones, or linezolid. ### Dosing and Duration - **Mupirocin ointment:** Apply a thin layer to affected areas **three times daily** for **7–10 days**. - **Cure rate:** 85–95% with appropriate topical therapy. - **Follow-up:** Review at 48 hours; if no improvement, switch to systemic antibiotic. [cite:Park 26e Ch 5; IAD Guidelines on Impetigo 2022] 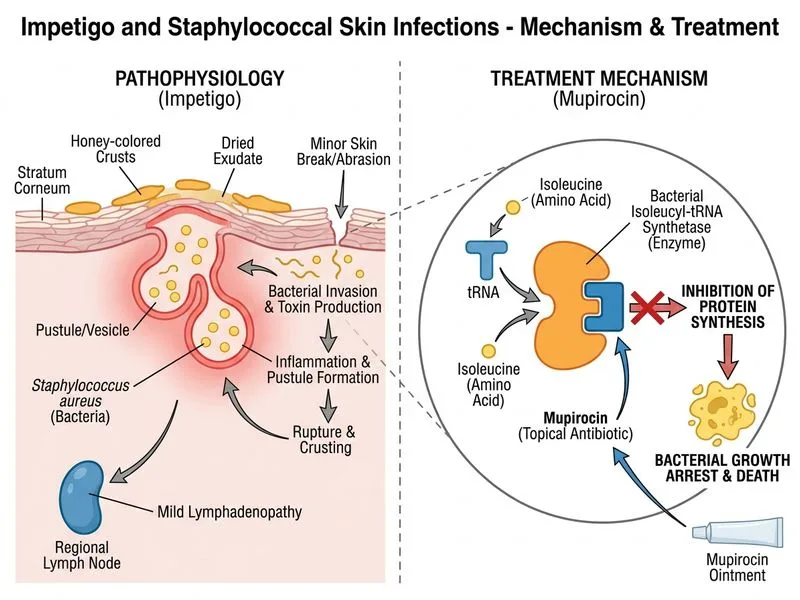
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.