## Management of Bullous Impetigo in Infants ### Clinical Context: Bullous Impetigo **Key Point:** Bullous impetigo accounts for ~30% of impetigo cases and is most common in neonates and infants. It is caused by *Staphylococcus aureus* producing exfoliative toxins (ETA and ETB), which cleave desmoglein-1 in the granular layer, leading to intra-epidermal acantholysis and blister formation. The infection remains **localized** (unlike SSSS, where toxins spread hematogenously). ### Why This Infant Requires Systemic Therapy | Feature | Non-Bullous Impetigo | Bullous Impetigo | |---------|----------------------|------------------| | **Age of onset** | 2–6 years | Neonates and infants | | **Lesion morphology** | Honey crusts | Flaccid bullae | | **Depth of infection** | Superficial (stratum corneum) | Intra-epidermal (granular layer) | | **Systemic involvement** | Minimal | Risk of dissemination | | **Treatment** | Topical antibiotics alone | Systemic antibiotics (± topical) | | **Risk of complications** | Low | Higher (sepsis, glomerulonephritis) | **High-Yield:** Bullous impetigo in infants requires **systemic antibiotics** because: 1. The infant is in a high-risk age group (immunologically immature) 2. Exfoliative toxins can cause widespread skin loss and fluid/electrolyte imbalance 3. Risk of secondary bacteremia and systemic infection is higher 4. Topical therapy alone is insufficient for intra-epidermal infection ### Antibiotic Selection **First-line systemic agent for bullous impetigo in a non-toxic infant:** Oral cephalexin (first-generation cephalosporin) or oral flucloxacillin — both provide excellent anti-staphylococcal coverage. Per standard dermatology and pediatric infectious disease guidelines (AAP Red Book; Rook's Dermatology), **oral cephalexin** is the preferred outpatient agent for non-MRSA bullous impetigo in a clinically stable infant. **Why IV flucloxacillin (Option C) is NOT the most appropriate initial management here:** - The infant is **afebrile and appears well** — no systemic toxicity - IV therapy is reserved for: systemic toxicity, extensive disease with fluid/electrolyte compromise, failure of oral therapy, or immunocompromised state - Initiating IV therapy in a stable, well-appearing infant is overtreatment and not the "most appropriate initial" step **Why topical mupirocin alone (Option A) is insufficient:** - Topical monotherapy is adequate only for non-bullous impetigo with limited lesions - Bullous impetigo in infants carries higher systemic risk; oral antibiotics are mandatory **Why amoxicillin-clavulanate alone (Option D) is suboptimal:** - While amoxicillin-clavulanate covers *S. aureus*, it is not the first-line agent for bullous impetigo - Cephalexin is preferred for its superior staphylococcal coverage and established safety profile in infants - Option D also lacks the topical adjunct **Clinical Pearl:** The combination of **topical mupirocin 2% plus oral cephalexin** (Option B) addresses both the local bacterial burden and the systemic risk. Mupirocin reduces autoinoculation and spread; cephalexin provides systemic anti-staphylococcal coverage appropriate for an outpatient, non-toxic infant. This is the standard of care per Fitzpatrick's Dermatology and AAP guidelines. ### Distinguishing Bullous Impetigo from SSSS | Feature | Bullous Impetigo | SSSS | |---------|-----------------|------| | **Toxin spread** | Local | Hematogenous (distant from infection site) | | **Nikolsky sign** | Negative | Positive | | **Fever/systemic toxicity** | Usually absent | Usually present | | **Culture of bullae** | Positive for *S. aureus* | Negative (toxin-mediated) | | **Management** | Oral antibiotics ± topical | IV anti-staphylococcal antibiotics | This infant has **positive bullae culture** and is **afebrile and well** — consistent with bullous impetigo, NOT SSSS. SSSS would require IV flucloxacillin, but that is not the diagnosis here. ### Treatment Duration and Follow-up - **Systemic antibiotic:** 7–10 days - **Topical antibiotic:** Continue until lesions healed (usually 7–10 days) - **Follow-up:** Reassess at 48 hours; if worsening, consider IV therapy or MRSA coverage (clindamycin, trimethoprim-sulfamethoxazole) - **Prevention:** Keep areas clean and dry; avoid sharing towels/clothing; trim infant's nails **Mnemonic: BULLOUS IMPETIGO IN INFANTS = Systemic + Topical** - **B**ullae with flaccid rupture → systemic therapy needed - **U**nder 1 year old → high-risk age group - **L**ocal + systemic therapy (mupirocin + cephalexin) - **L**ow toxicity → oral, not IV - **O**ral cephalexin is first-line - **U**se mupirocin topically as adjunct - **S**ystemic therapy mandatory (unlike non-bullous impetigo) *Reference: Fitzpatrick's Dermatology, 9th ed.; AAP Red Book 2021; Rook's Textbook of Dermatology, 9th ed.* 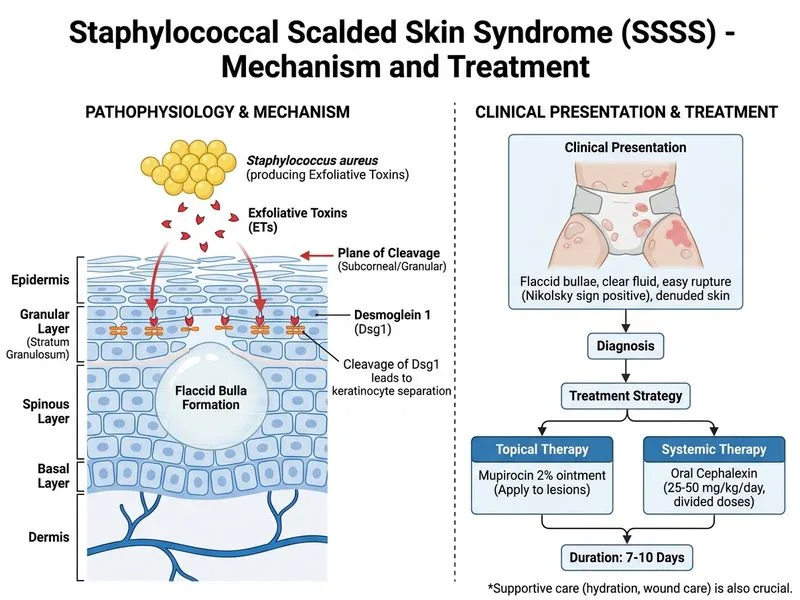
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.