## Diagnosis: Non-Bullous Impetigo ### Clinical Presentation Analysis **Key Point:** Non-bullous impetigo accounts for ~70% of all impetigo cases and is the most common form in India and tropical regions. The clinical triad present in this case: 1. **Honey-colored crusts** — pathognomonic for impetigo, especially non-bullous type 2. **Superficial pustules** — confined to the epidermis, not subepidermal 3. **Rapid progression** — papule → vesicle → pustule → crust over 3–5 days ### Microbiology & Gram Stain **High-Yield:** Gram-positive cocci in clusters = *Staphylococcus aureus*. This is the predominant pathogen in non-bullous impetigo (~80% of cases), especially in tropical climates. Group A Streptococcus (*Streptococcus pyogenes*) is the other common cause but appears as chains on Gram stain. ### Epidemiology & Risk Factors **Clinical Pearl:** This patient has classic risk factors: - Age 2–6 years (peak incidence) - Poor hygiene / crowded living (shared bedding) - Warm, humid climate (tropical region) - Minor skin trauma (abrasions on forearm/knee) - Contagious nature (sister infected 1 week prior) ### Comparison: Bullous vs. Non-Bullous Impetigo | Feature | Non-Bullous | Bullous | |---------|-------------|----------| | **Frequency** | 70% | 30% | | **Lesion type** | Pustules with crusts | Flaccid bullae | | **Crust color** | Honey-golden | Thin, transparent | | **Pathogen** | *S. aureus* (80%), *S. pyogenes* (20%) | *S. aureus* (phage group II, exfoliative toxin) | | **Depth** | Superficial (intraepidermal) | Subepidermal (subcorneal) | | **Scarring** | Rare | Rare | ### Why Gram Stain Confirms *S. aureus* Gram-positive cocci arranged in **clusters** (grape-like) = *Staphylococcus aureus*. In contrast, *Streptococcus pyogenes* appears as chains. **Mnemonic:** **CLUSTERS = STAPH** (Staphylococcus aureus clusters like grapes); **CHAINS = STREP** (Streptococcus chains like pearls). ### Management Implications **Key Point:** First-line treatment for non-bullous impetigo in India: - **Topical:** Mupirocin 2% ointment (3 times daily for 7 days) — for localized lesions - **Systemic:** Oral cephalexin or amoxicillin-clavulanate if extensive or failed topical therapy - **Isolation:** Until 48 hours after starting antibiotics to prevent spread [cite:Park 26e Ch 10] 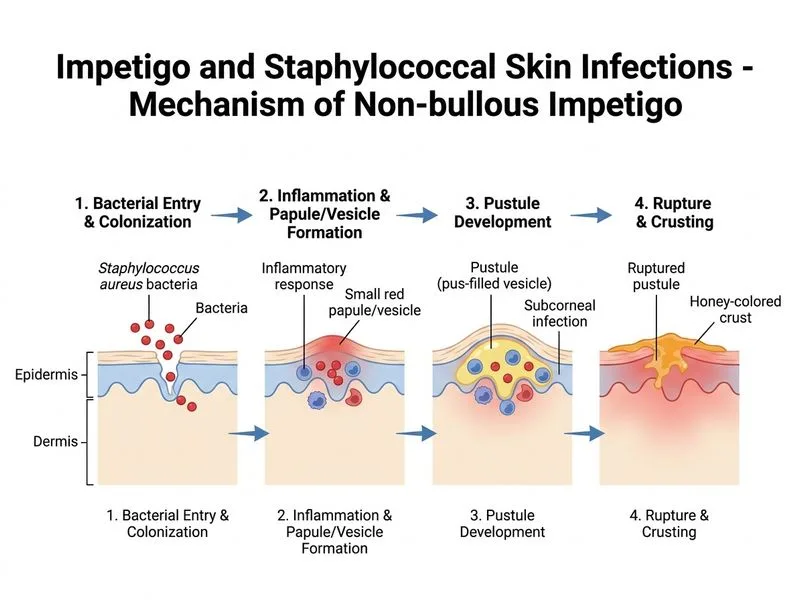
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.