## Diagnosis: Impetigo Secondary to Depilation Trauma ### Clinical Context & Pathogenesis **Key Point:** Impetigo commonly develops on sites of minor skin trauma, including abrasions from depilation, insect bites, eczema, and scratches. The depilatory cream caused microabrasions, creating a portal of entry for *Staphylococcus aureus*. ### Characteristic Features of Impetigo **High-Yield:** The clinical presentation matches non-bullous impetigo: - **Grouped lesions** — multiple pustules in close proximity - **Erosions with crusts** — rupture of pustules leaves shallow erosions - **Purulent exudate** — yellow-green drainage - **Surrounding erythema and edema** — inflammatory response - **Gram-positive cocci in clusters** — *Staphylococcus aureus* confirmed - **Afebrile, systemically well** — localized infection, no systemic toxicity ### Gram Stain Interpretation **Mnemonic:** **CLUSTERS = STAPH** — Gram-positive cocci in clusters = *Staphylococcus aureus*. This is the most common pathogen in impetigo, especially in adults with traumatized skin. ### Differential Diagnosis Exclusion | Feature | Impetigo | HSV-1/2 | VZV | Erysipeloid | |---------|----------|---------|-----|-------------| | **Vesicle grouping** | Grouped pustules | Grouped vesicles on erythematous base | Crops of vesicles | Urticarial plaques | | **Gram stain** | Gram+ cocci (clusters) | Negative | Negative | Gram+ rod | | **Prodrome** | None | Burning, tingling | Dermatomal pain | Localized | | **Systemic symptoms** | Rare | Possible (fever, malaise) | Possible (fever, malaise) | Rare | | **Recurrence** | No | Yes (latency) | Yes (dermatomal) | No | **Clinical Pearl:** The absence of vesicles on an erythematous base (typical of HSV) and the presence of erosions with purulent exudate point to bacterial impetigo, not viral infection. ### Why Depilation is a Risk Factor 1. **Mechanical trauma** — depilatory cream or waxing causes microabrasions 2. **Disruption of skin barrier** — compromised stratum corneum allows bacterial colonization 3. **Warm, moist environment** — intertriginous areas (thighs, abdomen) favor bacterial growth 4. **Inoculation** — *S. aureus* from normal flora or environment enters the wound ### Management **Key Point:** First-line treatment: - **Topical:** Mupirocin 2% ointment 3 times daily for 7–10 days (for localized lesions) - **Systemic:** Oral cephalexin 500 mg QID or amoxicillin-clavulanate if extensive - **Supportive:** Avoid further trauma, maintain hygiene, avoid depilation until healed - **Isolation:** Avoid skin-to-skin contact for 48 hours after starting antibiotics **High-Yield:** Topical antibiotics are first-line for localized impetigo; systemic antibiotics are reserved for extensive disease, facial involvement, or immunocompromised patients. [cite:Park 26e Ch 10; Harrison 21e Ch 124] 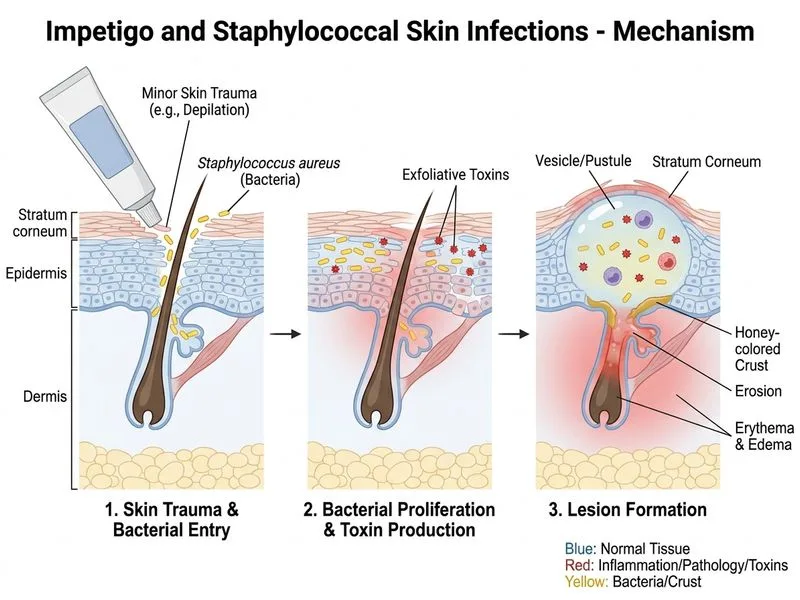
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.