## Diagnosis: Bullous Impetigo with MRSA ### Clinical Features **Key Point:** Bullous impetigo is characterized by flaccid bullae (not tense) with clear fluid that rupture easily, leaving thin transparent crusts. Nikolsky sign is **negative** (distinguishing it from pemphigus). **High-Yield:** Bullous impetigo is caused by exfoliative toxins (exfoliative toxin A or B) produced by *Staphylococcus aureus*, particularly phage group II strains. These toxins cause intraepidermal acantholysis at the granular layer. ### Microbiology Challenge: MRSA **Warning:** This patient has MRSA (methicillin-resistant *S. aureus*), which requires: - Avoidance of β-lactams (penicillins, cephalosporins) - Selection of agents with proven MRSA coverage ### Treatment Options Analysis | Agent | MRSA Coverage | Oral Bioavailability | Skin Penetration | Status | |-------|---------------|----------------------|------------------|--------| | Cloxacillin | No (β-lactam) | Good | Good | **Ineffective for MRSA** | | Linezolid | Yes (oxazolidinone) | Excellent (100%) | Excellent | **First-line for oral MRSA** | | Ceftriaxone | No (β-lactam) | IV only | Good | **Ineffective for MRSA** | | Vancomycin | Yes | Poor (IV only) | Moderate | **Reserved for severe/systemic** | **Key Point:** Linezolid is the preferred oral agent for MRSA skin infections because: 1. **100% oral bioavailability** — no need for IV access in ambulatory setting 2. **Excellent skin and soft tissue penetration** — achieves therapeutic levels in skin 3. **Proven efficacy** in MRSA impetigo and other skin infections 4. **Well-tolerated** in children with appropriate dosing ### Treatment Algorithm for MRSA Impetigo ```mermaid flowchart TD A[Bullous impetigo with MRSA]:::outcome --> B{Severity?}:::decision B -->|Localized,<br/>no systemic toxicity| C[Oral linezolid]:::action B -->|Extensive or<br/>systemic signs| D[IV vancomycin]:::action C --> E[Linezolid 10 mg/kg/day<br/>divided BID x 10-14 days]:::action D --> F[Vancomycin 15 mg/kg IV<br/>every 6 hours]:::action E --> G[Excellent oral absorption<br/>and skin penetration]:::outcome F --> G ``` **Clinical Pearl:** Although this child has mild fever, the infection is localized to skin without signs of systemic toxicity (no cellulitis, no lymphangitis). Oral linezolid is therefore appropriate and avoids the need for hospitalization and IV access. ### Why Not the Other Options? **Cloxacillin:** β-lactam; ineffective against MRSA (resistant by definition). **Ceftriaxone:** Third-generation cephalosporin; also a β-lactam and ineffective against MRSA. Additionally, it is IV-only and unnecessary for localized skin infection. **Vancomycin:** While effective for MRSA, it is reserved for: - Severe/invasive infections - Systemic toxicity - Inability to tolerate oral agents Vancomycin has poor oral bioavailability and is not absorbed from the GI tract; IV administration is required. For a localized, non-severe impetigo, linezolid is superior. 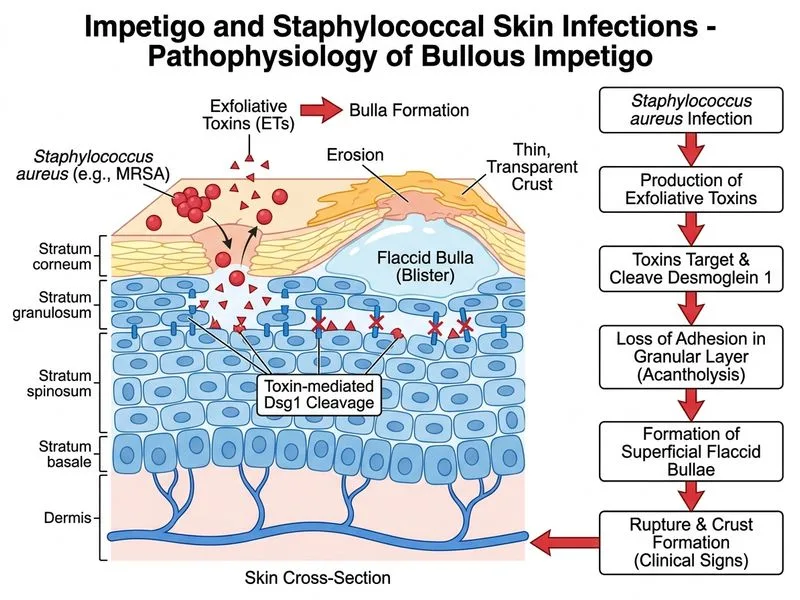
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.