## Investigation of Choice in Non-Bullous Impetigo **Key Point:** Gram stain and culture from the lesion is the gold standard for confirming bacterial impetigo and identifying the causative organism (Staphylococcus aureus or Streptococcus pyogenes). ### Why Gram Stain and Culture? 1. **Organism Identification** - Gram stain shows Gram-positive cocci in clusters (S. aureus) or chains (S. pyogenes) - Culture confirms the organism and allows antibiotic susceptibility testing (AST) - Essential in the era of MRSA to guide empiric therapy 2. **Antibiotic Susceptibility Testing** - Determines resistance patterns (β-lactamase, MRSA, etc.) - Guides choice between β-lactams, cloxacillin, or glycopeptides - Reduces treatment failure and prevents resistance spread 3. **Clinical Correlation** - Non-bullous impetigo (70% of cases) typically caused by S. aureus - Bullous impetigo caused by exfoliative toxin-producing S. aureus - Culture differentiates from other bacterial skin infections **High-Yield:** In India, MRSA prevalence in community impetigo is rising; culture-guided therapy is increasingly important. ### Specimen Collection - Swab the base of the lesion (not the crust alone) - Transport in sterile tube or culture medium - Best yield before topical antibiotics are applied **Clinical Pearl:** In uncomplicated non-bullous impetigo with typical presentation, empiric topical antibiotics (mupirocin) may be started; culture confirms diagnosis and guides escalation if needed. [cite:Fitzpatrick's Dermatology in General Medicine Ch 195] 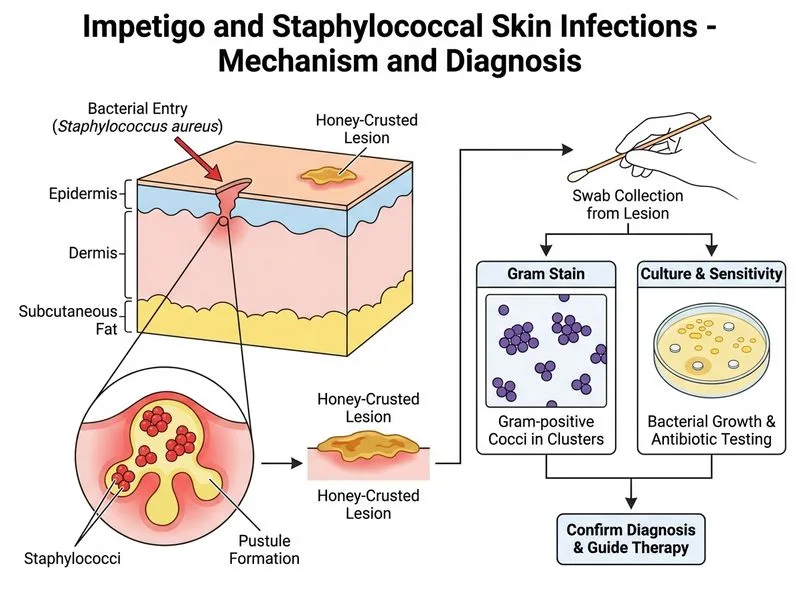
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.