## Clinical Diagnosis **Key Point:** This is non-bullous impetigo (most common form, ~70% of cases), characterized by honey-crusted lesions on exposed areas, typically following minor trauma or insect bites. ## Management Hierarchy for Impetigo | Presentation | First-line Treatment | Rationale | |---|---|---| | **Localized (< 5 lesions or < 2% BSA)** | Topical mupirocin 2% TDS | High efficacy, minimal systemic absorption, prevents spread | | **Localized with poor hygiene** | Topical mupirocin + oral antibiotic | Dual approach to reduce carriage | | **Generalized (> 5 lesions or > 2% BSA)** | Oral β-lactamase-resistant penicillin or cephalosporin | Systemic coverage for Staph aureus | | **Bullous impetigo** | Oral antibiotic ± topical | Deeper dermal involvement | ## Why Topical Mupirocin is Correct Here **High-Yield:** This patient has: - Localized lesions (2 sites only) - Non-bullous morphology - No systemic toxicity - No signs of cellulitis or deeper infection **Clinical Pearl:** Topical mupirocin achieves excellent local concentrations and eradicates *Staphylococcus aureus* and *Streptococcus pyogenes* from the lesion site and nares, reducing recurrence. It is the **gold standard for localized impetigo** in children [cite:Park 26e Ch 23]. **Mechanism:** Mupirocin inhibits bacterial isoleucyl-tRNA synthetase, halting protein synthesis. ## When to Escalate to Oral Antibiotics 1. Lesions > 5 in number or > 2% BSA 2. Bullous impetigo (risk of systemic spread) 3. Facial lesions near eyes/mouth (risk of orbital/perioral cellulitis) 4. Signs of cellulitis or lymphangitis 5. Immunocompromised host 6. Failed topical therapy after 5–7 days **Tip:** Always examine for signs of post-streptococcal sequelae (PSGN) in older children with impetigo caused by *S. pyogenes*; urinalysis at 2–3 weeks if high-risk. 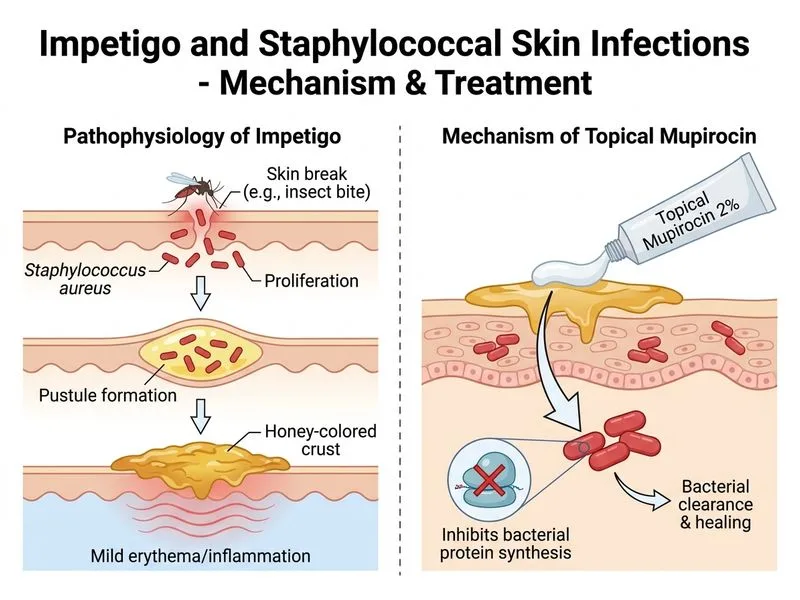
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.