## Non-Bullous Impetigo: Epidemiology and Clinical Features **Key Point:** Non-bullous impetigo accounts for ~90% of all impetigo cases and is most commonly caused by **Staphylococcus aureus** in contemporary practice, often with secondary colonization by *Streptococcus pyogenes*. The hallmark lesion is a **honey-crusted erosion** on an erythematous base. ### Epidemiological Shift in Causative Organisms **High-Yield:** Historically, *S. pyogenes* was the primary cause of impetigo globally. However, in the last 2–3 decades, *S. aureus* (including MRSA strains) has become the predominant pathogen in most regions, including India. This shift is clinically significant for antibiotic selection. ### Clinical Presentation of Non-Bullous Impetigo | Feature | Description | |---------|-------------| | **Lesion morphology** | Pustules → erosions with honey-colored crust | | **Base** | Erythematous, may have surrounding edema | | **Location** | Face (especially around nose and mouth), extremities, areas of minor trauma | | **Spread** | Centrifugal; highly contagious | | **Systemic symptoms** | Usually absent; regional lymphadenitis may occur | | **Healing** | Crusts fall off in 1–2 weeks; minimal scarring | ### Distinction from Bullous Impetigo **Warning:** Do not confuse non-bullous impetigo (honey crusts, superficial erosions) with bullous impetigo (flaccid bullae, intraepidermal split). The causative organism and toxin differ: - **Non-bullous:** *S. aureus* ± *S. pyogenes*; hyaluronidase, lipase, proteases - **Bullous:** *S. aureus* with exfoliative toxin; intraepidermal acantholysis **Clinical Pearl:** In Indian practice, empiric therapy for impetigo should cover *S. aureus* (including MRSA consideration based on local resistance patterns). Topical mupirocin is first-line for localized lesions; oral antibiotics (cephalosporin, amoxicillin-clavulanate, or fluoroquinolone) for extensive disease. 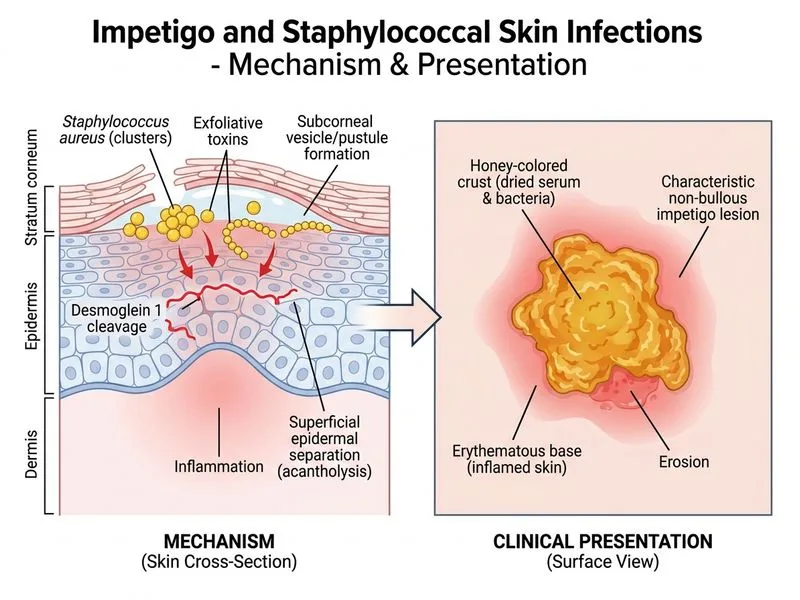
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.