## Diagnosis: Non-Bullous Impetigo (Staphylococcal) **Key Point:** The clinical presentation—flaccid bullae with honey-crusted erosions in a child—is pathognomonic for impetigo caused by *Staphylococcus aureus*. Gram stain showing gram-positive cocci in clusters confirms staphylococcal etiology. **High-Yield:** Impetigo is classified into two types: | Feature | Non-Bullous (70%) | Bullous (30%) | |---------|-------------------|---------------| | **Causative organism** | *S. aureus* (now most common) or *S. pyogenes* | *S. aureus* (exfoliative toxin) | | **Lesion morphology** | Vesicles → pustules → honey crusts | Flaccid bullae → erosions | | **Crust character** | Golden-yellow, adherent | Thin, easily ruptured | | **Age group** | 2–6 years (most common) | 2–5 years | | **Spread pattern** | Slower, localized | Rapid, can be widespread | **Clinical Pearl:** The "honey crust" (melicerious crust) is the hallmark of impetigo and distinguishes it from other bacterial infections. The ease of bullae rupture in this case points to bullous impetigo, a *S. aureus*–mediated condition via exfoliative toxins (ETA/ETB). ### First-Line Antibiotic Selection **Key Point:** For localized impetigo (< 5 lesions or limited body surface area), **topical antibiotics** (mupirocin) are preferred. However, for **generalized or bullous impetigo**, systemic antibiotics are indicated. Given the description of multiple lesions and bullae, **oral cephalexin** (a first-generation cephalosporin) is the first-line systemic agent: - Excellent *S. aureus* coverage (including MSSA) - Good skin penetration - Oral bioavailability - Safe in children - Dosing: 25–50 mg/kg/day divided into 4 doses **Mnemonic:** **SCAB** — *S. aureus*, *C*ephalexin, *A*ntibiotics, *B*acterial skin infection. ### Why This Diagnosis? 1. **Epidemiology:** *S. aureus* is now the leading cause of impetigo in most developed and developing countries, including India, replacing *S. pyogenes*. 2. **Gram stain:** Cocci in clusters = *Staphylococcus* (vs. *Streptococcus* = cocci in chains). 3. **Bullous morphology:** Exfoliative toxins produced by *S. aureus* cause intraepidermal acantholysis, leading to flaccid bullae. 4. **Age and setting:** School/dormitory exposure is a risk factor for rapid spread. [cite:Robbins 10e Ch 25] 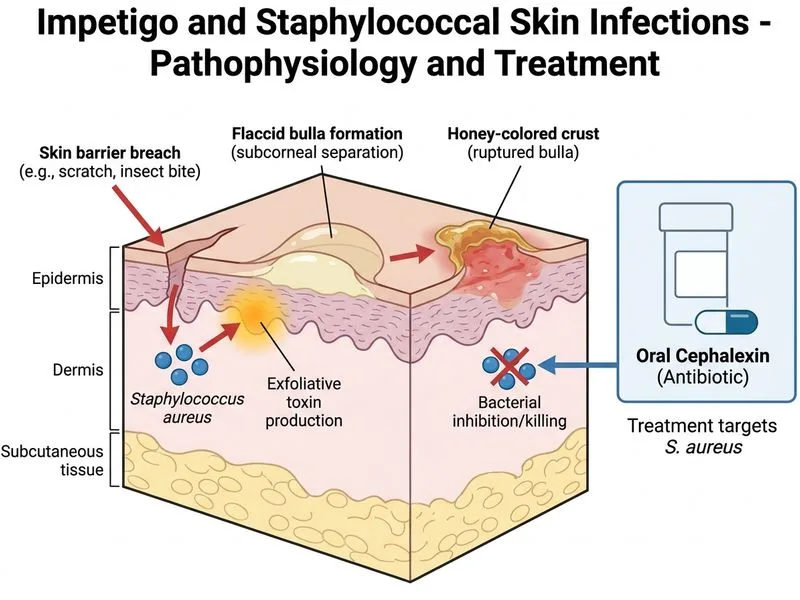
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.