## Clinical Assessment This case differs from the first question by the presence of **systemic signs**: - Fever (38.5°C) - Regional lymphadenopathy (cervical nodes) - Extensive lesions (legs and buttocks — likely >2% BSA) - Gram-positive cocci in clusters → *Staphylococcus aureus* or *Streptococcus pyogenes* These findings indicate **non-bullous impetigo with systemic involvement** — a step up in severity that requires oral antibiotics. ## Decision Algorithm: When to Escalate from Topical to Oral Therapy ```mermaid flowchart TD A[Impetigo with fever/lymphadenopathy]:::outcome --> B{Systemic signs present?}:::decision B -->|Fever, lymphadenopathy, extensive lesions| C[Oral antibiotics indicated]:::action B -->|No systemic signs, localized| D[Topical mupirocin sufficient]:::action C --> E{Suspected organism?}:::decision E -->|MSSA/Strep| F[Cephalexin or Amoxicillin-clavulanate]:::action E -->|MRSA suspected| G[Clindamycin or TMP-SMX]:::action F --> H[Monitor response at 48-72 hrs]:::action G --> H ``` ## Why Oral Antibiotics Are Now Needed **Key Point:** The presence of fever and cervical lymphadenopathy indicates systemic response to infection. This shifts management from topical-only to systemic therapy. **High-Yield:** Indications for oral antibiotics in impetigo: - Fever or systemic toxicity - Regional or generalized lymphadenopathy - Lesions affecting >2% BSA - Facial impetigo (risk of spread to eyes) - Immunocompromised patient - Failure of topical therapy after 5–7 days ## Antibiotic Selection: Cephalexin + Topical Mupirocin | Parameter | Cephalexin | Clindamycin | IV Ceftriaxone | |-----------|-----------|-----------|----------------| | **Indication** | First-line oral for MSSA/Strep | MRSA or allergy | Severe/invasive disease | | **Dose (child)** | 12.5–25 mg/kg QID | 10–13 mg/kg TID | 50–80 mg/kg/day | | **Spectrum** | MSSA, Strep, gram-positive | Anaerobes, MRSA, Strep | Broad (gram-pos, gram-neg) | | **Resistance risk** | Low | Moderate | Very low | | ***C. difficile* risk** | Very low | Higher | Higher | | **Oral bioavailability** | 90% | 90% | N/A (IV only) | **Clinical Pearl:** Cephalexin 250 mg QID (or 12.5–25 mg/kg/day divided QID) is the gold standard first-line oral antibiotic for community-acquired impetigo with systemic signs. It covers both *S. aureus* (MSSA) and *Streptococcus pyogenes*. ## Why Combination Therapy (Oral + Topical)? **Tip:** Adding topical mupirocin to oral cephalexin: 1. Provides higher local concentration at lesion sites 2. Reduces bacterial shedding and transmission 3. Accelerates clinical healing 4. Is recommended in guidelines for extensive or systemic impetigo ## Gram Stain Interpretation Gram-positive cocci in clusters = *Staphylococcus aureus* (most likely in this context). Gram-positive cocci in chains = *Streptococcus pyogenes*. Both are covered by cephalexin; clindamycin is reserved for MRSA or penicillin allergy. ## Why NOT IV Therapy? **Warning:** Intravenous antibiotics are NOT indicated for non-bullous impetigo unless: - Signs of invasive infection (cellulitis, abscess, necrotizing fasciitis) - Severe systemic toxicity (sepsis, shock) - Immunocompromised host with disseminated disease This child has uncomplicated impetigo with reactive lymphadenopathy and low-grade fever — oral therapy is sufficient. 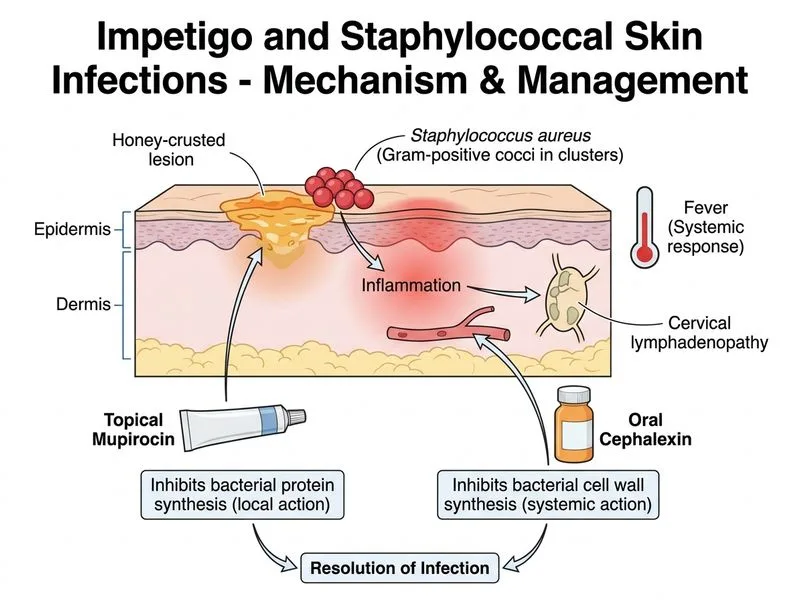
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.