## Distinguishing Non-Bullous from Bullous Impetigo ### Clinical Presentation Comparison | Feature | Non-Bullous Impetigo | Bullous Impetigo | |---------|---------------------|------------------| | **Primary lesion** | Erythematous macule → pustule → crust | Flaccid bullae (thin-walled) | | **Crust character** | Honey-colored, thick, adherent | Purulent fluid beneath intact blister | | **Blister presence** | Absent; crusts form directly on skin | Present; precedes erosion | | **Causative organism** | *S. aureus* (75%), *S. pyogenes* (25%) | *S. aureus* only (exfoliative toxins) | | **Frequency** | 70% of all impetigo cases | 30% of all impetigo cases | | **Healing** | Leaves post-inflammatory hyperpigmentation | Leaves erosions, minimal scarring | **Key Point:** Non-bullous impetigo is defined by the **absence of a blister stage** — lesions progress directly from pustule to characteristic honey-colored crust without an intervening flaccid blister. ### Pathophysiology **Non-bullous:** - Direct invasion of superficial epidermis - Inflammatory response → pustule formation - Crust = dried serum + pus + bacteria **Bullous:** - *S. aureus* produces exfoliative toxins (exfoliatin A/B) - Toxins cleave desmoglein-1 in granular layer - Intraepidermal acantholysis → flaccid blister - Blister roof ruptures → erosion with thin crust **High-Yield:** The **honey crust without preceding blister** is the pathognomonic discriminator of non-bullous impetigo. Bullous impetigo always shows the blister stage first. **Clinical Pearl:** Non-bullous impetigo is more common (70%) and more contagious; bullous impetigo is more likely to be caused by *S. aureus* phage group II strains. ### Why This Matters - Non-bullous: topical antibiotics often sufficient - Bullous: requires systemic antibiotics due to deeper involvement - Bullous: higher risk of systemic toxicity (SSSS in neonates) [cite:Fitzpatrick's Dermatology 9e Ch 193] 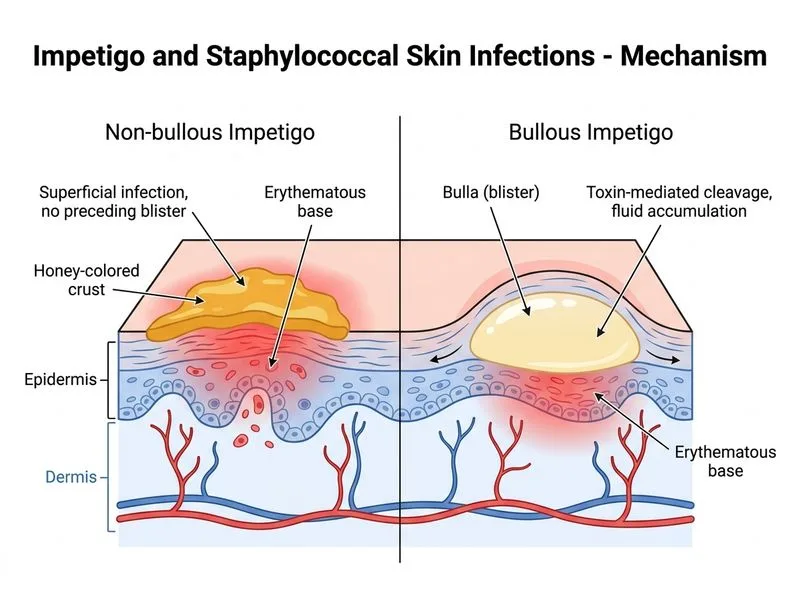
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.