## Diagnosis: Ulcerative Colitis ### Clinical Presentation The patient presents with the classic triad of ulcerative colitis (UC): - Bloody diarrhea with mucus - Abdominal cramping - Weight loss and systemic inflammation (elevated ESR, CRP) ### Key Distinguishing Features | Feature | Ulcerative Colitis | Crohn's Disease | |---------|-------------------|------------------| | **Distribution** | Continuous, starts rectally | Skip lesions, patchy | | **Depth** | Mucosa and submucosa only | Transmural | | **Granulomas** | Absent | Present in 30–50% | | **Crypt distortion** | Present | Present | | **Fistulas/strictures** | Rare | Common | **Key Point:** The **continuous mucosal inflammation limited to rectum and sigmoid colon** is pathognomonic for UC. Crohn's disease typically shows skip lesions (patchy distribution with normal intervening mucosa). **High-Yield:** Absence of granulomas on biopsy strongly favors UC over Crohn's disease. Granulomas are found in only 30–50% of Crohn's cases but are virtually absent in UC. ### Pathologic Findings in UC 1. **Mucosal and submucosal inflammation** — neutrophilic infiltration 2. **Crypt distortion** — loss of normal architecture 3. **Crypt abscess** — neutrophils within crypt lumens 4. **Absence of transmural involvement** — distinguishes from Crohn's 5. **No granulomas** — key negative finding **Clinical Pearl:** Fecal calprotectin >250 µg/g indicates active IBD; this patient's level of 450 µg/g confirms significant mucosal inflammation. ### Why UC and Not Crohn's? - Continuous distribution (not skip lesions) - Limited to colon (not small bowel involvement) - Mucosal-only disease (not transmural) - No granulomas on histology - Rectal involvement (UC typically starts here and spreads proximally) 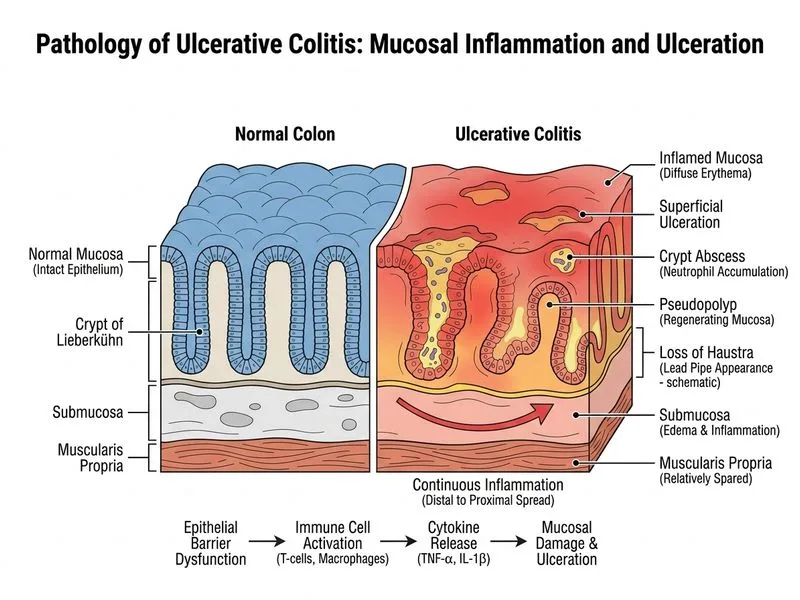
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.