## Diagnosis of Inflammatory Bowel Disease **Key Point:** Colonoscopy with multiple mucosal biopsies from both affected and unaffected areas is the gold standard for diagnosing IBD and differentiating ulcerative colitis from Crohn's disease. ### Why Colonoscopy with Biopsies? Colonoscopy allows: 1. **Direct visualization** of mucosal inflammation, ulceration, and distribution pattern 2. **Histopathological confirmation** — biopsies show crypt distortion, chronic inflammation, and crypt abscesses 3. **Differentiation** between UC (continuous, superficial colonic involvement) and CD (patchy, transmural involvement) 4. **Assessment of disease extent and severity** — essential for prognosis and treatment planning ### Histological Features on Biopsy | Feature | Ulcerative Colitis | Crohn's Disease | |---------|-------------------|------------------| | **Distribution** | Continuous, limited to colon | Patchy, skip lesions | | **Depth** | Mucosal/submucosal | Transmural | | **Crypt distortion** | Marked | Moderate | | **Granulomas** | Absent | Present (30–50%) | | **Fissuring ulcers** | Absent | Present | **Clinical Pearl:** Multiple biopsies (≥2 from colon, ≥1 from terminal ileum if accessible) increase diagnostic yield and reduce sampling error. **High-Yield:** The combination of **clinical presentation + endoscopic findings + histology** is required for definitive IBD diagnosis. No single investigation is sufficient. ### Role of Other Investigations - **Fecal calprotectin:** Useful for screening and monitoring inflammation, but NOT diagnostic - **CT enterography:** Excellent for assessing small bowel involvement and complications (strictures, fistulas) in CD, but not first-line for diagnosis - **Capsule endoscopy:** Reserved for suspected small bowel CD when colonoscopy/ileoscopy is non-diagnostic; not first-line [cite:Robbins 10e Ch 17] 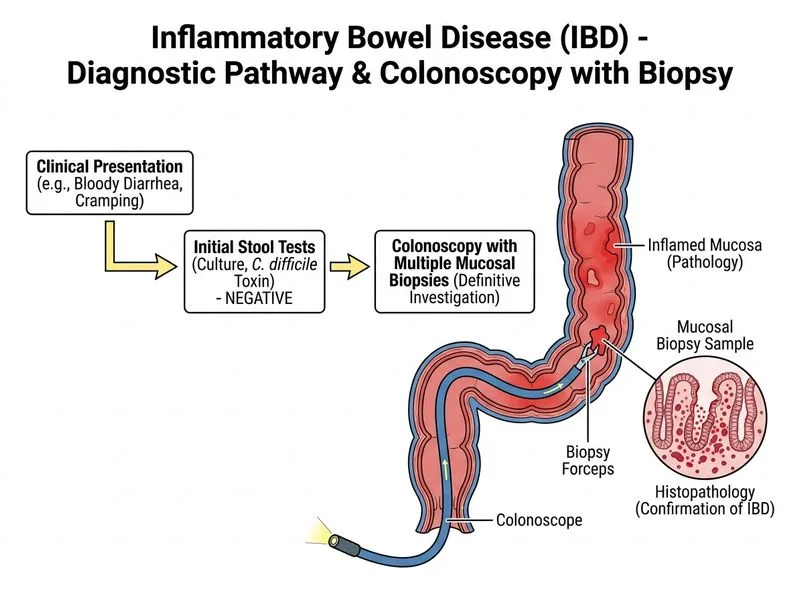
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.