## Diagnosis: Ulcerative Colitis ### Clinical Presentation The patient presents with the classic triad of ulcerative colitis: - **Bloody diarrhea** with mucus (hallmark feature) - **Continuous colonic involvement** without skip lesions - **Systemic inflammation** (elevated ESR, CRP, high fecal calprotectin) ### Key Pathological Features | Feature | Ulcerative Colitis | Crohn Disease | |---------|-------------------|---------------| | **Distribution** | Continuous, colon only | Skip lesions, any part of GI tract | | **Depth of inflammation** | Mucosa and submucosa | Transmural (full thickness) | | **Crypt distortion** | Present | Present | | **Granulomas** | Absent | Present in 30–50% | | **Fissuring ulcers** | Rare | Common | | **Haustra** | Loss of haustra (lead pipe appearance) | Preserved initially | **Key Point:** The absence of granulomas on histology, continuous mucosal inflammation limited to the colon, and loss of haustra are diagnostic of ulcerative colitis. ### Colonoscopic Findings - Friability and bleeding of mucosa - Continuous inflammation from rectum proximally - No skip lesions - Loss of normal vascular pattern and haustra **High-Yield:** Fecal calprotectin >250 μg/g indicates active IBD; this patient's value of 420 confirms active disease and helps exclude IBS. ### Laboratory Correlation - **Elevated inflammatory markers** (ESR 68, CRP 12) support IBD - **Microcytic anemia** (Hb 9.2) from chronic blood loss - **Fecal calprotectin** is a neutrophil-derived protein; high levels indicate mucosal inflammation **Clinical Pearl:** In ulcerative colitis, the inflammation is limited to the mucosa and submucosa, which is why extraintestinal manifestations (arthritis, uveitis, erythema nodosum) are less common than in Crohn disease. 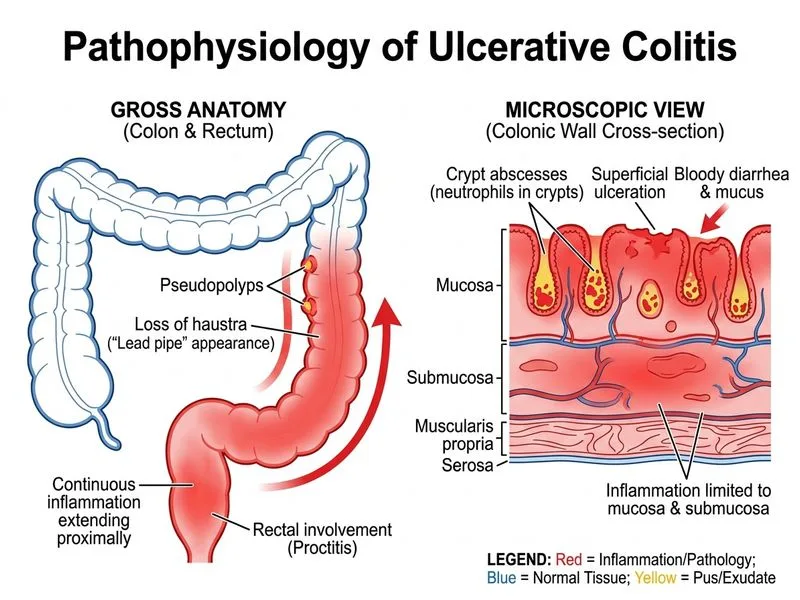
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.