## Distinguishing Histopathology of IBD ### Key Pathological Differences **Key Point:** Non-caseating granulomas in a transmural distribution are pathognomonic for Crohn's disease and are absent in ulcerative colitis. ### Comparative Table | Feature | Crohn's Disease | Ulcerative Colitis | | --- | --- | --- | | **Depth of inflammation** | Transmural (all layers) | Mucosal and submucosal only | | **Granulomas** | Non-caseating (30–50% of cases) | Absent | | **Distribution** | Skip lesions (patchy) | Continuous, starts at rectum | | **Crypt abscess** | Present | Present | | **Fissuring ulcers** | Characteristic | Superficial ulcers | | **Fibrosis & strictures** | Common | Rare | ### Clinical Correlation **High-Yield:** While crypt abscess, goblet cell loss, and crypt distortion occur in both diseases, **transmural inflammation with non-caseating granulomas** is the single most specific histological finding that definitively identifies Crohn's disease. **Clinical Pearl:** Granulomas are found in approximately 30–50% of Crohn's disease biopsies; their absence does not exclude the diagnosis, but their presence is virtually diagnostic of Crohn's. ### Why This Matters The transmural nature of Crohn's inflammation explains its clinical complications: - Fistula formation (penetrating through all layers) - Stricture formation (fibrosis in deeper layers) - Perforation risk In contrast, ulcerative colitis is limited to mucosa and submucosa, explaining why perforation and fistulas are rare. [cite:Robbins 10e Ch 17] 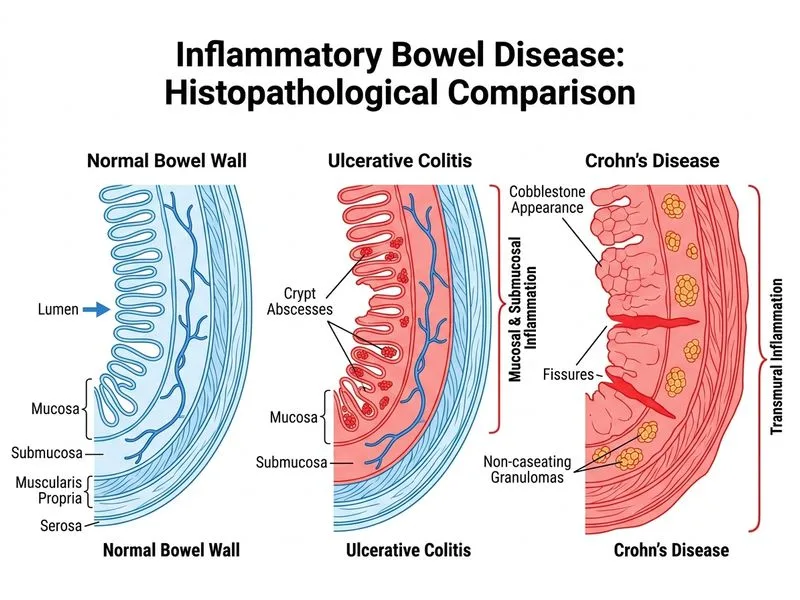
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.