## Investigation of Choice for Crohn's Disease Complications **Key Point:** Contrast-enhanced CT abdomen and pelvis is the investigation of choice for suspected intra-abdominal complications in Crohn's disease (abscess, fistula, perforation, obstruction). It provides rapid diagnosis, guides intervention, and assesses disease extent. ### Clinical Context: Acute Crohn's Complication The clinical presentation—acute pain, fever, palpable mass, elevated inflammatory markers—suggests an intra-abdominal complication, most likely an **abscess** (common in Crohn's disease, especially with terminal ileal involvement). ### Why CT with IV Contrast? 1. **Sensitivity and specificity**: CT is 90–95% sensitive for detecting abscesses >2 cm and can identify fistulas, strictures, and perforation. 2. **Rapid diagnosis**: Essential in acute presentation with fever and peritoneal signs. 3. **Guides intervention**: Allows assessment of abscess size, location, and accessibility for percutaneous drainage. 4. **Staging**: Evaluates transmural disease, mesenteric fat stranding, and complications. 5. **Therapeutic planning**: Determines whether medical management, percutaneous drainage, or surgery is needed. ### Comparison of Imaging Modalities in Acute Crohn's | Modality | Role | Limitation in Acute Setting | |---|---|---| | **CT with IV contrast** | Gold standard for acute complications (abscess, perforation, obstruction) | Radiation; contrast contraindicated in severe renal impairment | | **Abdominal X-ray** | Detects free air (perforation), obstruction signs | Poor sensitivity for soft tissue; cannot diagnose abscess or fistula | | **MR enterography** | Excellent for small bowel disease, fistula mapping, non-invasive | Time-consuming; not ideal for acute/unstable patients; less sensitive for acute abscess | | **Ultrasound** | Portable, no radiation, good for fluid collection | Operator-dependent; poor in obese patients; limited assessment of transmural disease | **Clinical Pearl:** In acute Crohn's with fever and mass, percutaneous drainage of abscess under CT guidance is often the first step, followed by medical optimisation. This "drain and treat" approach avoids emergency surgery in many cases. **High-Yield:** CT enterography (with oral and IV contrast) is standard for chronic disease assessment and small bowel mapping in stable patients. However, in acute presentations with fever and peritoneal signs, standard CT abdomen/pelvis with IV contrast is faster and more appropriate. **Warning:** Do not delay imaging waiting for MRI in an acutely unwell patient. CT is faster and more sensitive for acute abscess in this clinical context. **Mnemonic: ACUTE-CT** — **A**bscess detection, **C**omplications (fistula, perforation), **U**rgent diagnosis, **T**ransmural assessment, **E**xtra-luminal disease — all best shown on **CT**. 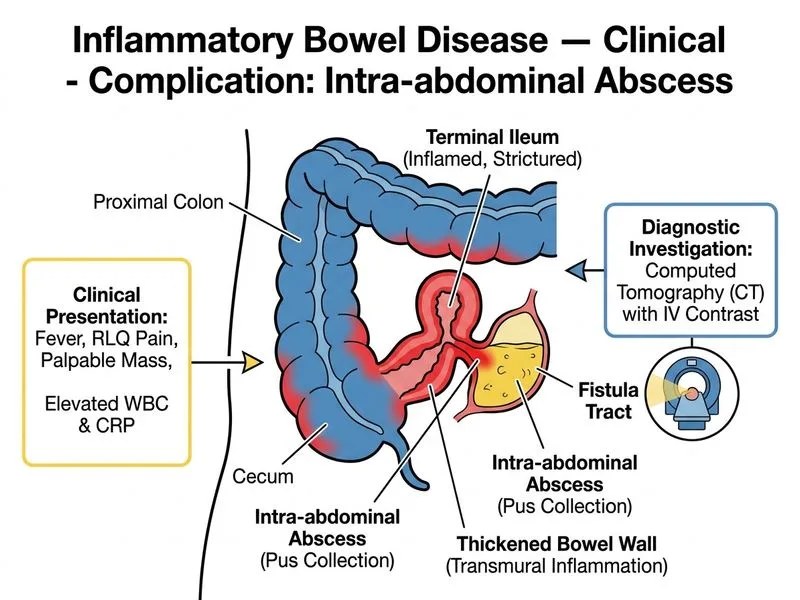
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.