## Clinical Assessment This patient presents with **severe ulcerative colitis** (SCCF criteria): - Stool frequency >6/day with blood - Systemic toxicity (fever, tachycardia) - Anemia (Hb 9.2) - Hypoalbuminemia (2.8 g/dL) indicating malnutrition - Elevated inflammatory markers (CRP 8.5) - Endoscopic severity (continuous ulceration, loss of haustra) ## Management Algorithm for Severe UC ```mermaid flowchart TD A[Severe UC confirmed]:::outcome --> B{Fulminant features?}:::decision B -->|Toxic megacolon, perforation, shock| C[Emergency colectomy]:::urgent B -->|No fulminant signs| D[IV corticosteroids + supportive care]:::action D --> E[Admit to hospital]:::action E --> F[Optimize fluids, electrolytes, nutrition]:::action F --> G{Response at 3-5 days?}:::decision G -->|Yes| H[Continue IV steroids, taper oral]:::action G -->|No| I[Rescue therapy: infliximab or ciclosporin]:::action ``` ## Why IV Hydrocortisone Is Correct **Key Point:** Severe UC with systemic toxicity requires **immediate hospitalization and IV corticosteroids**, not escalation of 5-ASA monotherapy. **High-Yield:** Standard induction therapy for severe UC: - IV hydrocortisone 100 mg 6-hourly (or methylprednisolone 40–60 mg daily) - Supportive care: IV fluids, electrolyte repletion, blood transfusion if Hb <7 - Prophylactic antibiotics if signs of sepsis - NPO or liquid diet; TPN if prolonged **Clinical Pearl:** Response is assessed at **3–5 days**. If no improvement → rescue therapy (infliximab or ciclosporin). If deterioration or fulminant signs → urgent colectomy. **Warning:** Do NOT delay steroids or attempt outpatient management in severe disease. Mortality risk increases with delayed intervention. ## Rationale for Rejecting Other Options See **whyEachDistractorIsWrong** below. [cite:Harrison 21e Ch 297] 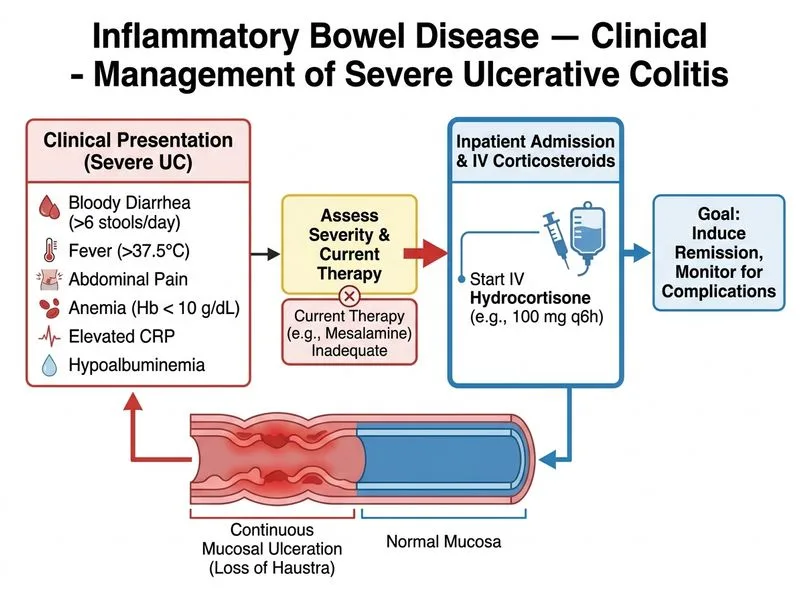
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.