## Distinguishing Ulcerative Colitis from Crohn's Disease ### Depth of Inflammation: The Key Discriminator **Key Point:** The hallmark distinguishing feature of ulcerative colitis (UC) is that inflammation is **limited to the mucosa and submucosa**, whereas Crohn's disease is **transmural** (involves all layers including muscularis propria and serosa). ### Comparison Table | Feature | Ulcerative Colitis | Crohn's Disease | |---------|-------------------|------------------| | **Depth of inflammation** | Mucosa + submucosa only | Transmural (all layers) | | **Distribution** | Continuous, rectum to proximal colon | Skip lesions, patchy | | **Fistulas/sinuses** | Absent | Common | | **Crypt abscesses** | Present | May be present | | **Cobblestone appearance** | Absent | Present | | **Perianal disease** | Rare | Common (30–40%) | ### Why This Matters Clinically **Clinical Pearl:** Transmural inflammation in Crohn's disease explains its complications: fistulas, strictures, and abscess formation. Mucosal-limited disease in UC explains why colectomy is curative—the disease does not extend beyond the colon. **High-Yield:** On histology, transmural inflammation with non-caseating granulomas (seen in ~30–50% of Crohn's biopsies) is pathognomonic for Crohn's disease. UC never shows transmural disease or granulomas. ### Why Other Options Are Misleading - **Crypt abscesses & distortion:** Both UC and Crohn's can show these; not discriminatory. - **Absence of perianal disease:** While perianal fistulas are *more common* in Crohn's, they are not universally present; UC can rarely have perianal involvement. - **Elevated fecal calprotectin:** Both conditions elevate this marker; it reflects mucosal inflammation, not disease type. [cite:Harrison 21e Ch 295] 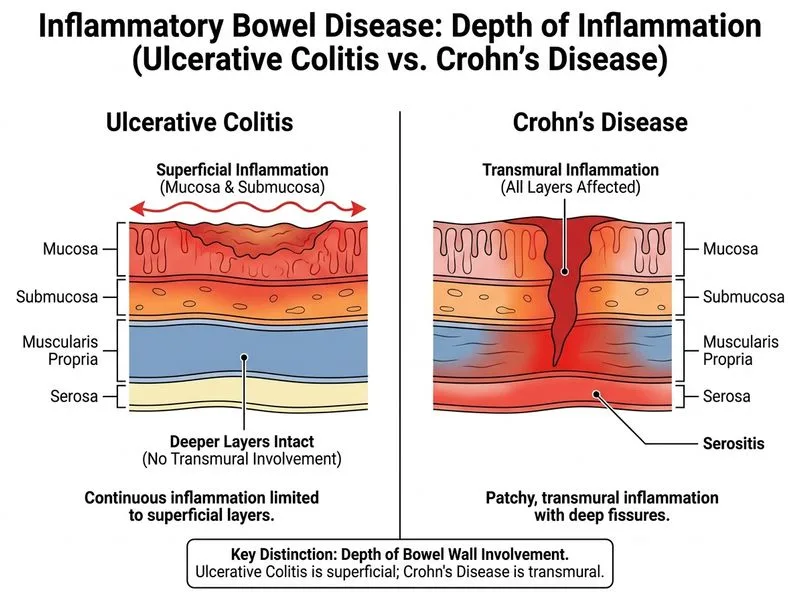
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.