## Investigation of Choice: Colonoscopy with Mucosal Biopsy ### Clinical Context This patient presents with an acute severe flare of ulcerative colitis (Truelove–Witts criteria: >6 bloody stools/day, fever >37.8°C, Hb <10.5 g/dL, CRP >30 mg/L, tachycardia). Importantly, **there are no clinical signs of toxic megacolon** (no abdominal distension, no absent bowel sounds, no haemodynamic instability), and stool cultures including C. difficile are negative — making colonoscopy both safe and the most informative next step. ### Why Colonoscopy with Biopsy is Correct **Key Point:** In acute UC flares without evidence of toxic megacolon or perforation, limited flexible sigmoidoscopy/colonoscopy with mucosal biopsy is the investigation of choice to assess disease severity, extent, and guide immediate management decisions (corticosteroids vs. biologics vs. surgery). This is endorsed by ECCO (European Crohn's and Colitis Organisation) guidelines and Harrison's Principles of Internal Medicine (21e, Ch. 297). **High-Yield:** Colonoscopy during acute IBD flares (in the absence of toxic megacolon): - Directly visualises mucosal ulceration, friability, and loss of vascular pattern — enabling endoscopic severity grading (Mayo score) - Permits histological grading and rules out superimposed infection (CMV colitis, which can mimic/complicate severe UC and requires specific antiviral therapy) - Identifies extent of disease (critical for surgical planning if needed) - Guides escalation of therapy: mesalamine → corticosteroids → biologics (infliximab/ciclosporin) → colectomy - Perforation risk in experienced hands during acute (non-fulminant) UC is low (~0.1–0.3%); the absence of toxic megacolon signs here makes the procedure safe **Clinical Pearl:** The key safety caveat is to **first exclude toxic megacolon** before proceeding to colonoscopy. In this patient, the absence of abdominal distension, haemodynamic compromise, or radiological colonic dilation makes colonoscopy appropriate and superior to plain X-ray alone. ### Why Other Options Are Suboptimal | Investigation | Limitation in This Context | |---|---| | **Abdominal X-ray** | Useful to screen for toxic megacolon (transverse colon >6 cm) or perforation, but this patient lacks clinical features of toxic megacolon. X-ray is insensitive for mucosal disease and does not guide therapy beyond ruling out one complication. It is a reasonable adjunct but not the single most appropriate investigation to assess severity and guide management. | | **CT enterography** | Optimised for small-bowel Crohn's disease and fistulae; less sensitive for mucosal detail in UC; does not provide tissue diagnosis; reserved for suspected complications (perforation, abscess, obstruction). | | **Faecal calprotectin** | A useful non-invasive marker for monitoring remission and predicting relapse, but does NOT grade endoscopic severity, guide acute inpatient management, or rule out CMV superinfection. It is a monitoring tool, not an acute severity assessment tool. | **Mnemonic — SCOPE for acute IBD flare:** - **S** = Severity grading (visual + histology) - **C** = Complications ruled out (no megacolon → colonoscopy safe) - **O** = Obtain biopsies (rule out CMV, confirm IBD) - **P** = Predict prognosis (extent, depth of ulceration) - **E** = Escalate therapy (based on findings) [cite: Harrison 21e Ch. 297; ECCO Guidelines on UC Management 2022] 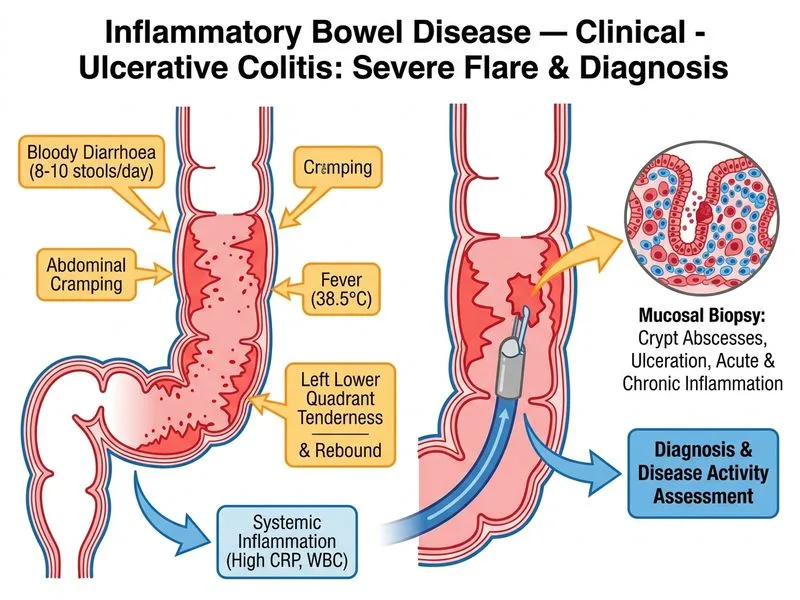
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.