## Clinical Scenario Assessment This patient presents with **acute severe ulcerative colitis** (Truelove and Witts criteria: >6 stools/day with blood, systemic toxicity with fever, anemia, and elevated inflammatory markers). She has failed conventional therapy (mesalamine + azathioprine) and is now in relapse. ## Management of Acute Severe UC **Key Point:** Acute severe UC is a medical emergency requiring hospitalization and intensive therapy. The patient meets criteria for fulminant disease and requires IV corticosteroids as first-line therapy, with early consideration of rescue therapy (anti-TNF agents or cyclosporine) if no response within 3–5 days. ### Rationale for IV Corticosteroids 1. **First-line therapy** for acute severe UC: IV methylprednisolone 500 mg–1 g daily or IV hydrocortisone 100 mg 6-hourly 2. **Rapid onset** of action in severe inflammation 3. **Bypass enteral absorption** issues in severe colitis 4. Response rate: 50–75% within 5–7 days ### Early Anti-TNF Consideration **High-Yield:** Current evidence (ECCO, ACG, ASGE guidelines) recommends **early anti-TNF therapy** (infliximab or adalimumab) in acute severe UC, particularly in: - Patients with prior immunosuppressive failure (as in this case) - High-risk features (young age, extensive disease, severe inflammation) - Predicted poor responders to corticosteroids alone **Clinical Pearl:** Delaying anti-TNF therapy in severe UC increases risk of colectomy. Early escalation (within 3–5 days of IV steroid initiation if inadequate response) improves outcomes. ### Why NOT Surgical Consultation First? Surgery is reserved for: - Fulminant colitis with toxic megacolon or perforation (no imaging evidence here) - Failed medical therapy after 7–10 days of intensive treatment - Uncontrolled sepsis or hemodynamic instability This patient requires a trial of intensive medical therapy first. ```mermaid flowchart TD A["Acute Severe UC<br/>(>6 stools/day + blood + toxicity)"]:::outcome --> B["Admit to hospital<br/>IV fluids, NPO, monitoring"]:::action B --> C["IV Corticosteroids<br/>(methylprednisolone 500 mg-1 g daily)"]:::action C --> D{"Response at day 3-5?"}:::decision D -->|"Yes (improving stool frequency,<br/>CRP declining)"|E["Continue IV steroids<br/>Transition to oral"]:::action D -->|"No (persistent diarrhea,<br/>worsening inflammation)"|F["Add Anti-TNF agent<br/>(infliximab 5 mg/kg IV)"]:::action F --> G{"Response at day 7?"}:::decision G -->|"Yes"|E G -->|"No"|H["Surgical consultation<br/>Consider colectomy"]:::urgent ``` ## Summary: Next Step **Initiate IV corticosteroids immediately** (methylprednisolone or hydrocortisone) with **early anti-TNF therapy** (infliximab) planned for day 3–5 if inadequate response. This is the standard-of-care escalation pathway for acute severe UC in a patient who has failed conventional therapy. [cite:Harrison 21e Ch 297] 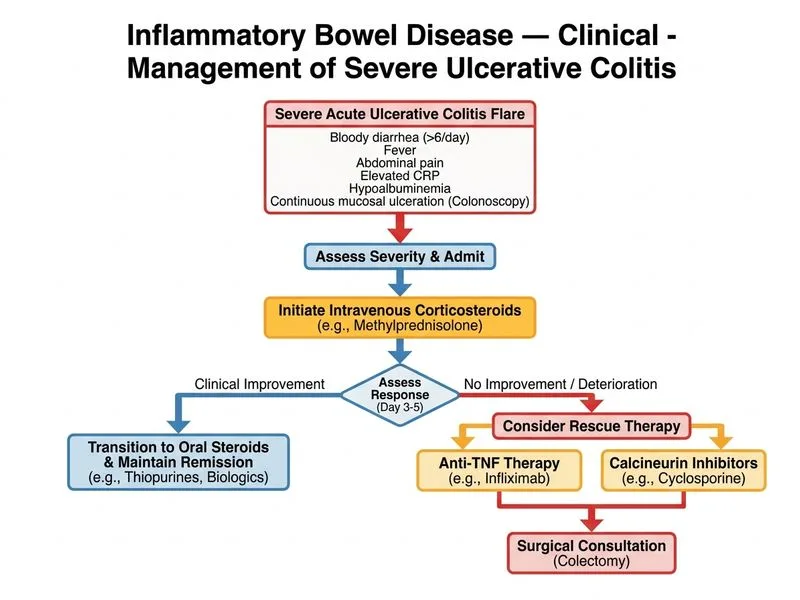
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.