## Clinical Presentation Analysis This patient presents with acute onset right-sided weakness affecting the face, arm, and leg equally, along with dysarthria — a classic **internal capsule/basal ganglia syndrome**. The CT head reveals a **hyperdense lesion** in the left basal ganglia region, which is the radiological hallmark of **intracerebral hemorrhage (ICH)**, not ischemic stroke. ### Radiological Key Point **Key Point:** On non-contrast CT: - **Hyperdense lesion** (bright white, 50–80 HU) = **acute blood/hemorrhage** - **Hypodense lesion** (dark, < 20 HU) = ischemia/infarction - **Isodense** = subacute blood or edema A hyperdense lesion in the basal ganglia in the context of acute neurological deficits is **intracerebral hemorrhage** until proven otherwise. This is a critical distinction because thrombolysis is **absolutely contraindicated** in hemorrhagic stroke. ### Anatomical Basis The basal ganglia (putamen) is the single most common site of hypertensive intracerebral hemorrhage (~35% of ICH), supplied by lenticulostriate arteries — small perforating vessels highly susceptible to hypertensive damage. Hemorrhage here compresses the adjacent internal capsule, producing contralateral hemiparesis with facial involvement and dysarthria. ### Management Algorithm for Acute ICH | Step | Action | |------|--------| | 1 | Confirm hemorrhage on CT (done) | | 2 | Assess hematoma size, location, neurological status | | 3 | Neurosurgical consultation for potential evacuation | | 4 | BP control, reversal of anticoagulation if applicable | | 5 | ICU monitoring and supportive care | **High-Yield:** For basal ganglia/putaminal hemorrhage with significant neurological deficits (3/5 weakness, dysarthria), the **most appropriate immediate next step** is **craniotomy for hematoma evacuation** (neurosurgical intervention), particularly when there is substantial neurological compromise. AHA/ASA 2022 ICH guidelines (Class IIb) support surgical evacuation for accessible supratentorial hematomas with neurological deterioration. ### Why Craniotomy / Hematoma Evacuation Is the Next Step 1. **CT confirms hemorrhage:** Hyperdense lesion = acute blood — thrombolysis is absolutely contraindicated 2. **Significant neurological deficit:** 3/5 weakness with dysarthria indicates substantial hematoma effect on the internal capsule 3. **Basal ganglia location:** Putaminal hemorrhages with mass effect and neurological deterioration are candidates for surgical evacuation per AHA/ASA ICH guidelines 4. **Guideline-based:** Harrison's Principles of Internal Medicine (21e, Ch 371) and AHA/ASA 2022 ICH guidelines recommend surgical evacuation for accessible supratentorial hematomas with neurological deterioration ### Why Each Distractor Is Suboptimal | Option | Why It's Wrong | |--------|---------------| | IV thrombolysis with alteplase (A) | **Absolutely contraindicated** in hemorrhagic stroke — would dramatically worsen the hemorrhage and is potentially fatal | | MRI with DWI/perfusion (B) | While MRI provides additional detail, CT has already confirmed hemorrhage — delaying for MRI is inappropriate when immediate neurosurgical intervention is indicated | | Oral aspirin 325 mg + observation (C) | Antiplatelet therapy is contraindicated in acute ICH; it impairs platelet function and worsens bleeding | **Clinical Pearl:** The single most important step in acute stroke management is distinguishing ischemic from hemorrhagic stroke via CT. A hyperdense basal ganglia lesion = hemorrhage = thrombolysis contraindicated. Never administer alteplase without confirming the absence of hemorrhage on CT. [cite: Harrison's Principles of Internal Medicine 21e, Ch 371; AHA/ASA 2022 ICH Guidelines] 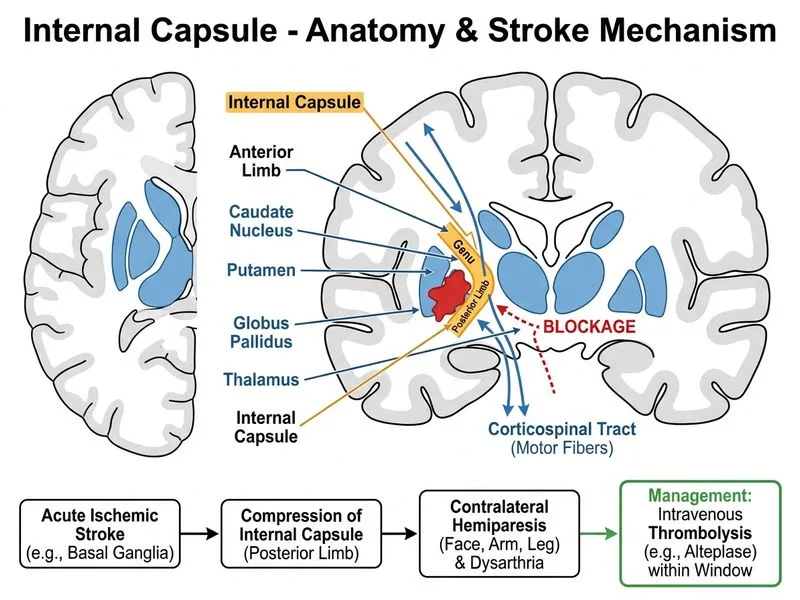
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.