## Clinical Context This patient presents with **acute small bowel obstruction** with clinical and radiological evidence of a transition zone. The vital signs are stable and there is no evidence of perforation (no free air). The clinical presentation is classic for mechanical obstruction. ## Management Algorithm for Acute Small Bowel Obstruction ```mermaid flowchart TD A[Acute SBO suspected]:::outcome --> B{Signs of perforation?}:::decision B -->|Yes: free air, peritonitis| C[Immediate laparotomy]:::urgent B -->|No| D{Vital signs stable?}:::decision D -->|Unstable/septic| E[Resuscitate + urgent surgery]:::urgent D -->|Stable| F[Nasogastric decompression]:::action F --> G[IV fluids, electrolyte correction]:::action G --> H[CT abdomen with oral/IV contrast]:::action H --> I{Complete obstruction?}:::decision I -->|Yes| J[Surgical consultation]:::action I -->|No/Partial| K[Conservative management trial]:::action ``` ## Why Nasogastric Tube + IV Fluids + CT Abdomen? **Key Point:** In **stable patients with acute SBO without peritonitis**, the standard approach is: 1. **Nasogastric decompression** — relieves distension, reduces vomiting, allows assessment of output 2. **IV fluid resuscitation** — corrects dehydration and electrolyte abnormalities (especially K^+^ loss from vomiting) 3. **CT abdomen with oral and IV contrast** — gold standard imaging to: - Confirm obstruction and identify transition zone - Determine **completeness** of obstruction (partial vs. complete) - Identify **etiology** (adhesion, hernia, malignancy, volvulus) - Assess for complications (ischemia, perforation) **High-Yield:** CT has **95% sensitivity and specificity** for mechanical SBO and guides management: partial obstruction may resolve with conservative care; complete obstruction requires surgery. **Clinical Pearl:** Plain radiographs (as shown here) are insensitive for etiology and cannot reliably distinguish partial from complete obstruction. CT is the next logical step after initial resuscitation. ## Why NOT Immediate Laparotomy? Patient is stable, no peritoneal signs, no free air. Surgery is indicated only after imaging confirms complete obstruction or if patient deteriorates. ## Why NOT Ultrasound? Ultrasound has poor sensitivity in acute obstruction due to bowel gas. It may assess wall thickness but cannot reliably determine obstruction level or etiology. ## Why NOT Barium Enema? Barium is contraindicated in suspected small bowel obstruction (risk of impaction). Barium enema is used for **colonic obstruction**, not ileal obstruction. CT is superior. 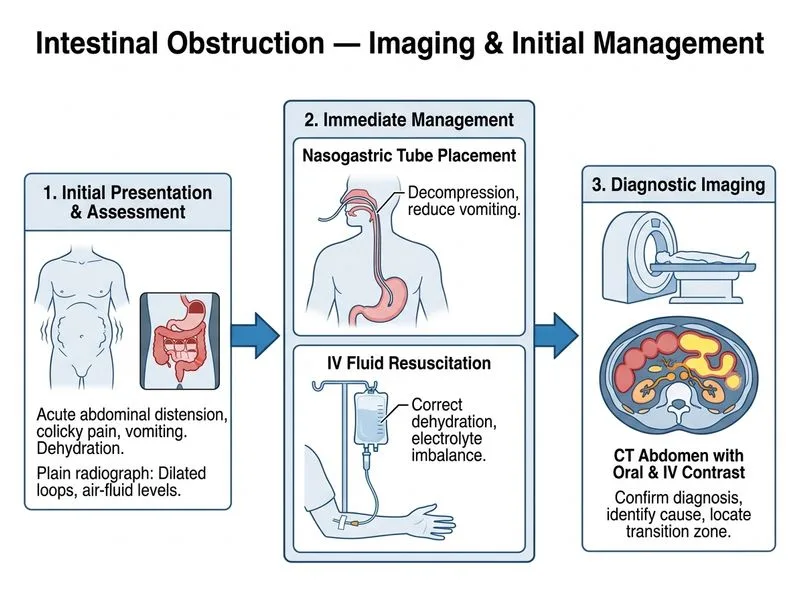
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.