## Clinical Context This patient has **adhesive small bowel obstruction** (most common cause in developed countries, accounting for 60–75% of cases). The imaging shows: - Transition zone in proximal ileum - Collapsed distal bowel - No free air, ascites, or wall thickening - **No signs of strangulation or ischemia** ## Adhesive Obstruction: Conservative vs. Surgical Management ```mermaid flowchart TD A[Adhesive SBO on imaging]:::outcome --> B{Signs of strangulation?}:::decision B -->|Yes: wall thickening, ascites, mesenteric edema| C[Urgent laparotomy]:::urgent B -->|No| D{Complete obstruction?}:::decision D -->|Yes + clinical deterioration| E[Surgical consultation]:::action D -->|No/Partial + stable| F[Nasogastric decompression]:::action F --> G[IV fluids + electrolyte correction]:::action G --> H[Observation 24-48 hours]:::action H --> I{Improvement?}:::decision I -->|Yes: decreased pain, reduced output| J[Continue conservative care]:::action I -->|No: worsening distension/pain| K[Laparotomy]:::urgent ``` ## Why Conservative Management (NG Tube + IV Fluids + Observation)? **Key Point:** **Adhesive obstruction resolves spontaneously in 60–80% of cases** with nasogastric decompression and supportive care alone. Surgery is reserved for: - Failure to resolve within 24–48 hours - Signs of strangulation (fever, peritonitis, elevated lactate) - Clinical deterioration **High-Yield:** This patient has: - ✓ Afebrile status - ✓ No peritoneal signs (mild tenderness only) - ✓ No imaging signs of ischemia (no wall thickening, ascites, or mesenteric edema) - ✓ Stable vital signs → **All criteria for trial of conservative management are met.** **Clinical Pearl:** The **"adhesion score"** on CT predicts success of conservative management: - Low-grade adhesions (transition zone, collapsed distal bowel, no ischemia) → 70–80% resolve with NG decompression - High-grade adhesions (thick-walled loops, ascites, mesenteric edema) → higher surgical rate ## Nasogastric Tube Specifics - Relieves distension and vomiting - Allows monitoring of output (decreasing output suggests resolution) - Reduces intraluminal pressure - **Serial clinical examination** is key: improvement in pain, distension, and NG output within 24–48 hours predicts success ## Why NOT Immediate Laparotomy? No signs of strangulation or complete obstruction with deterioration. Adhesiolysis carries risk of bowel injury and re-adhesion formation. Conservative management should be trialed first. ## Why NOT Oral Contrast Study? Oral contrast is contraindicated in suspected **complete obstruction** (risk of impaction). This patient's imaging already confirms obstruction; further oral contrast adds no diagnostic value and delays conservative management. ## Why NOT Percutaneous Drainage? There is no loculated fluid collection on imaging. Drainage is indicated only for abscess or significant ascites contributing to obstruction—neither is present here. 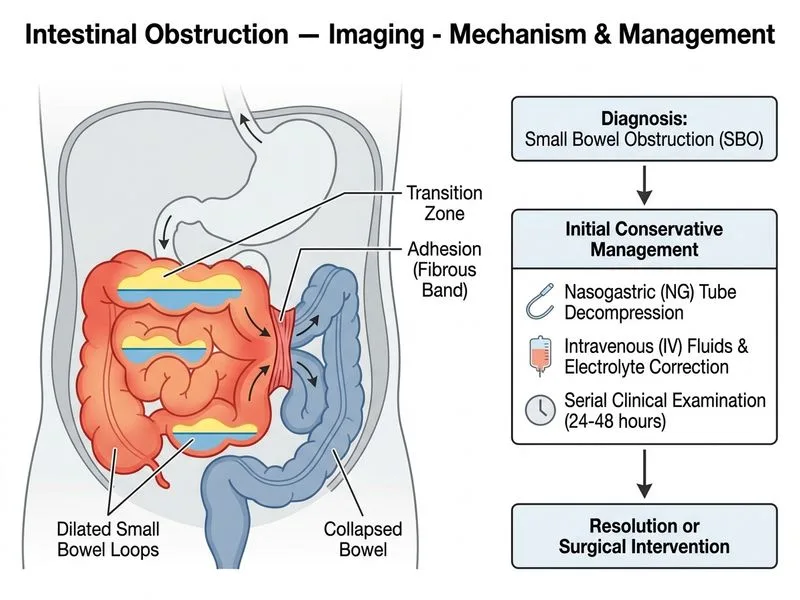
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.