## Clinical Scenario Analysis This patient presents with **recurrent partial small bowel obstruction** due to **postoperative adhesions** (history of appendicectomy, imaging shows tethered mesentery and focal adhesion with transition point). ## Imaging Findings Interpretation **Key Point:** The combination of: - Clustered small bowel loops ("concertina" pattern) - Tethered mesentery - Focal adhesion at transition zone - Stable hemodynamics ...is classic for **adhesive obstruction**, which resolves spontaneously in 60–80% of cases with conservative management. **High-Yield:** **Partial obstruction** (patient has had symptoms for 3 months, suggesting intermittent blockage) has a much higher spontaneous resolution rate than complete obstruction. ## Management Algorithm for Adhesive Small Bowel Obstruction ```mermaid flowchart TD A[Small bowel obstruction on imaging]:::outcome --> B{Clinical stability?}:::decision B -->|Hemodynamically unstable, peritonitis, complete obstruction| C[Exploratory laparotomy]:::urgent B -->|Stable, partial obstruction, no peritonitis| D[Conservative management]:::action D --> E[NGT decompression]:::action E --> F[IV fluids + electrolyte correction]:::action F --> G[Serial clinical exam over 48-72 hours]:::action G --> H{Improvement?}:::decision H -->|Yes| I[Discharge with dietary advice]:::outcome H -->|No| J[Exploratory laparotomy]:::action C --> K[Adhesiolysis ± resection]:::action ``` ## Rationale for Conservative Management **Key Point:** In **partial adhesive obstruction** with **hemodynamic stability**, the first-line approach is **conservative management** because: 1. **High spontaneous resolution rate** (60–80% resolve within 48–72 hours) 2. **Adhesiolysis carries morbidity** — risk of bowel perforation, enterotomy, and formation of new adhesions 3. **Recurrent episodes** suggest chronic partial obstruction, not acute complete obstruction **Clinical Pearl:** The "3-month history of recurrent episodes" is the key clinical clue — this patient has had multiple episodes that resolved spontaneously, making surgical intervention for the current episode premature. ## Conservative Management Protocol | Component | Rationale | |-----------|----------| | **NGT decompression** | Reduces proximal bowel distension, relieves symptoms, prevents aspiration | | **IV fluids + electrolytes** | Corrects dehydration and hypokalemia from vomiting | | **NPO status** | Allows bowel rest and reduces intraluminal pressure | | **Serial examination** | Detects signs of peritonitis, perforation, or worsening obstruction | | **Observation 48–72 hours** | Allows time for adhesion to lyse spontaneously | **Warning:** Do NOT give oral contrast (barium or water-soluble) in acute obstruction — risk of impaction and worsening obstruction. Oral contrast is used only in **suspected partial obstruction with stable imaging** to confirm passage and rule out complete obstruction (not applicable here, as imaging already shows obstruction). ## Indications for Urgent Laparotomy **High-Yield:** Proceed to surgery if: - **Peritoneal signs** (rebound, guarding, rigidity) - **Hemodynamic instability** (shock, tachycardia refractory to fluids) - **Failure to improve** after 48–72 hours of conservative management - **Imaging signs of strangulation** (closed-loop obstruction, ischemia) - **Complete obstruction** with no passage of flatus/stool This patient has NONE of these — hence conservative management is appropriate. 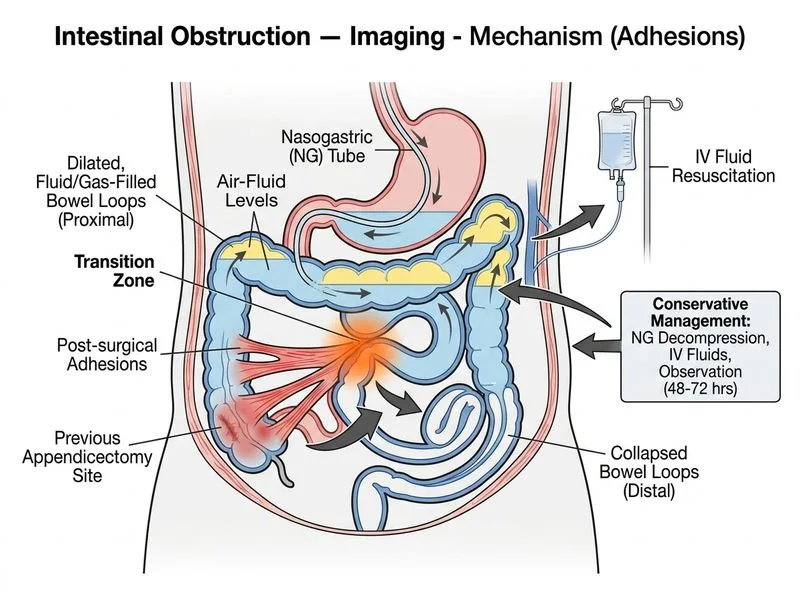
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.