## Investigation of Choice for Bacterial Meningitis **Key Point:** In a patient with clinical signs of meningitis (fever, headache, neck stiffness, Kernig's sign), the gold standard confirmatory test is **cerebrospinal fluid (CSF) analysis via lumbar puncture**. Blood cultures should be obtained first to identify the causative organism. **High-Yield:** The diagnostic sequence in suspected meningitis is: 1. Blood cultures (before antibiotics if possible) 2. Empiric broad-spectrum antibiotics (do NOT delay for imaging) 3. Lumbar puncture with CSF analysis (cell count, glucose, protein, Gram stain, culture, PCR) 4. Imaging (CT/MRI) only if contraindications to LP exist (papilloedema, focal neurological signs, immunocompromise) **Clinical Pearl:** In India, empiric therapy with ceftriaxone (or cefotaxime) + vancomycin ± ampicillin (for Listeria coverage in elderly/immunocompromised) should be started immediately after blood cultures, without waiting for imaging or LP results. **Warning:** Do NOT perform imaging before LP in uncomplicated meningitis — this delays diagnosis and treatment. Imaging is reserved for cases with contraindications to LP. ## CSF Findings in Bacterial Meningitis | Parameter | Bacterial | Viral | Tuberculous | |-----------|-----------|-------|-------------| | Cell count | 100–10,000 (PMN predominant) | 10–1,000 (lymphocyte predominant) | 100–500 (lymphocyte predominant) | | Glucose | <40 mg/dL (CSF:blood ratio <0.4) | Normal (>40 mg/dL) | Low (20–40 mg/dL) | | Protein | 100–500 mg/dL | 50–100 mg/dL | 100–500 mg/dL | | Gram stain | Positive in 60–90% | Negative | Negative | | Culture | Positive in 80–90% | Negative | Positive in 50–80% | [cite:Harrison 21e Ch 381] 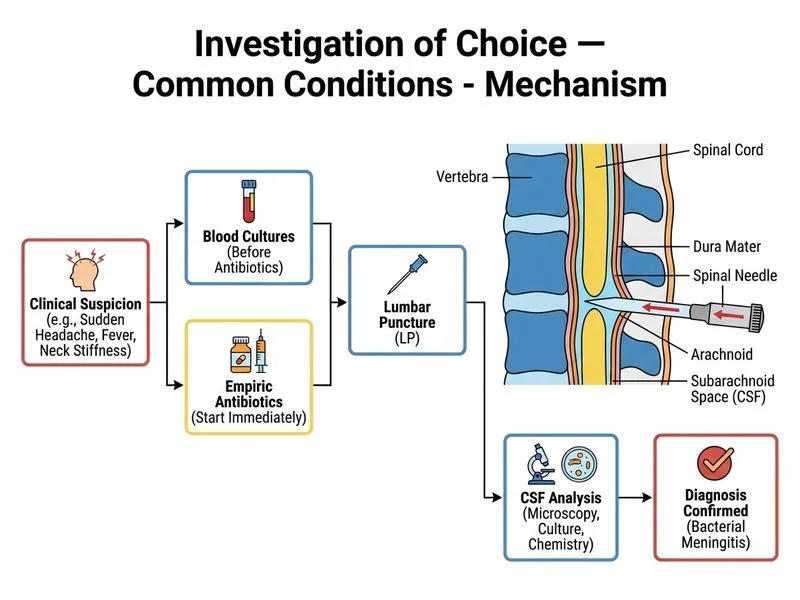
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.