## Investigation of Choice for Acute Subdural Hematoma **Key Point:** Non-contrast CT head is the gold standard and first-line imaging modality for acute subdural hematoma because it is rapid, widely available, and highly sensitive for detecting acute blood. ### Why Non-Contrast CT? 1. **Speed of acquisition** — Critical in acute neurological emergencies; CT is performed in <5 minutes 2. **High sensitivity for acute blood** — Appears hyperdense (bright) on CT due to high iron content of hemoglobin 3. **No contraindications** — Unlike MRI, no metal implant concerns in emergency settings 4. **Guides immediate management** — Rapid diagnosis allows urgent neurosurgical consultation and evacuation if indicated ### Characteristic CT Findings in Acute SDH | Feature | Appearance | | --- | --- | | **Acute (0–3 days)** | Hyperdense (white), crescent-shaped, does not cross suture lines | | **Subacute (3–20 days)** | Isodense to brain, may be missed on standard CT | | **Chronic (>20 days)** | Hypodense (dark), often bilateral | **High-Yield:** Acute subdural hematoma appears as a **crescent-shaped hyperdense collection** that **does NOT cross the midline** (unlike epidural hematoma, which is lens-shaped and does not cross suture lines). ### Why Other Modalities Are Not First-Line - **MRI brain:** Takes 30–45 minutes; contraindicated if metallic implants present; reserved for chronic SDH or when CT is equivocal - **Skull X-ray:** Low sensitivity; cannot detect intracranial blood; useful only to rule out skull fracture (not diagnostic for SDH) - **Transcranial Doppler:** Functional assessment tool; cannot visualize blood collections; not diagnostic **Clinical Pearl:** In a patient with acute altered consciousness and focal deficits, do NOT wait for MRI — perform non-contrast CT immediately and proceed to neurosurgery if SDH is confirmed. 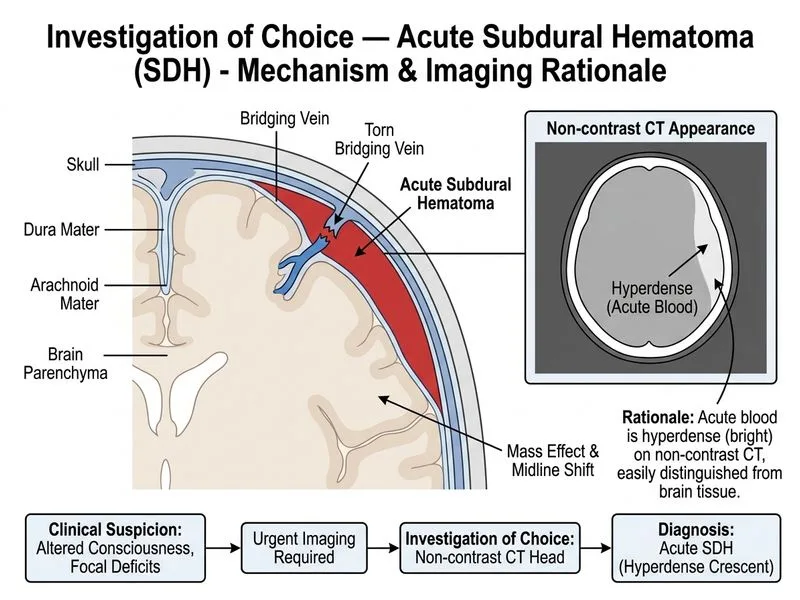
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.