## Clinical Context This patient has clinical features highly suspicious for acute pulmonary embolism (PE): acute dyspnea, pleuritic chest pain, hypoxia, and a wedge-shaped opacity on CXR (classic for pulmonary infarction). The next step is **definitive imaging**, not further blood tests or delayed imaging. ## Investigation Algorithm for Suspected PE ```mermaid flowchart TD A[Suspected PE: dyspnea + hypoxia<br/>+ wedge opacity on CXR]:::outcome --> B{Hemodynamically stable?}:::decision B -->|Yes| C[CTPA is first-line imaging]:::action B -->|No| D[Consider bedside echo<br/>for RV strain]:::action C --> E{CTPA result}:::decision E -->|PE confirmed| F[Start anticoagulation]:::action E -->|PE excluded| G[Investigate alternative diagnosis]:::action D --> H[If RV dysfunction suspected<br/>consider thrombolysis]:::urgent ``` ## Key Point: **CT pulmonary angiography (CTPA) is the gold standard for diagnosing PE** in hemodynamically stable patients. It has >95% sensitivity and specificity for central and segmental PEs. ## High-Yield: - **CTPA** is the investigation of choice for suspected PE in stable patients - **D-dimer** is useful for **ruling out** PE in low-risk patients (high negative predictive value), NOT for confirming it - **V/Q scan** is reserved for patients with: - Renal insufficiency (contrast contraindication) - Severe contrast allergy - Pregnancy (lower radiation dose) - Normal baseline CXR (V/Q more interpretable) - **Anticoagulation should NOT be delayed** while awaiting imaging if clinical suspicion is very high and imaging is not immediately available, but in this case CTPA is the appropriate next step ## Clinical Pearl: The wedge-shaped opacity (Hampton hump) is pathognomonic for **pulmonary infarction**, which occurs when PE causes distal airway occlusion with subsequent alveolar hemorrhage. This finding significantly increases the likelihood of PE and warrants immediate CTPA. ## Why Not D-dimer First? **D-dimer is a screening tool, not a diagnostic tool.** It has: - High sensitivity (~95%) but **low specificity** (~30–40%) - Elevated in many conditions: infection, inflammation, malignancy, recent surgery, pregnancy - Useful only to **exclude** PE in low-risk patients (negative D-dimer + low clinical probability = PE ruled out) - **NOT useful to confirm** PE (positive D-dimer does not diagnose PE) In this case with high clinical suspicion and radiological findings, D-dimer adds no value; CTPA is indicated immediately. ## Why Not V/Q Scan? V/Q scan is **not first-line** for PE diagnosis in modern practice because: - Lower sensitivity and specificity than CTPA - Many indeterminate results - Requires normal baseline CXR for interpretation (this patient has an abnormal CXR) - Longer acquisition time V/Q is reserved for specific scenarios (renal failure, contrast allergy, pregnancy). [cite:Harrison 21e Ch 298; Fleischner Society Guidelines 2019] 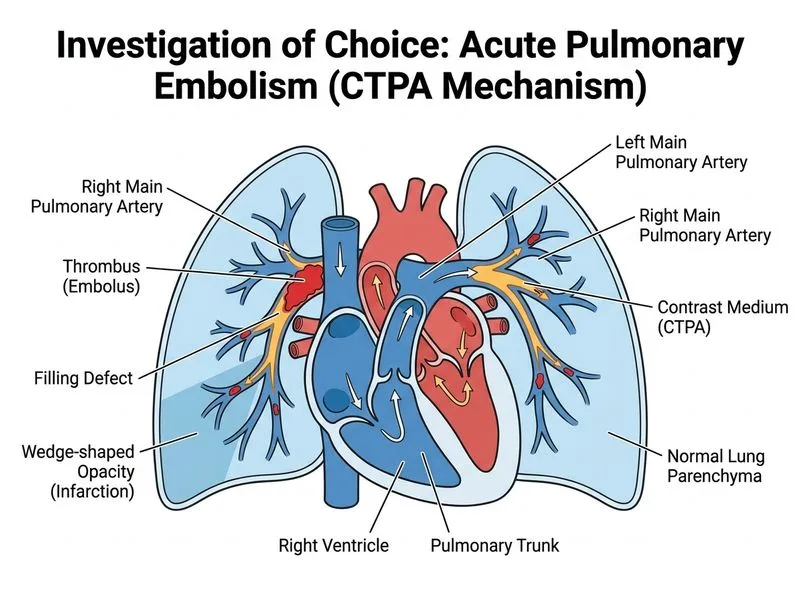
Sign up free to access AI-powered MCQ practice with detailed explanations and adaptive learning.